ADD & ADHD - Attention Deficit Disorder
& Attention Deficit Hyperactivity Disorder
|

|
Learning Discoveries Psychological Services
Rosemary Boon Registered Psychologist
M.A.(Psych), Grad. Dip. Ed. Studies (Sch.Counsel), Grad. Dip. Ed., B.Sc., MAPS, AACNEM. |
|
Telephone: Sydney (+61 2) 9637 9998
Facsimile: Sydney (+61 2) 9637 8799 |
Email: rboon@learningdiscoveries.org |
Postal Address:-
P.O. Box 9047
Harris Park NSW 2150
Australia |

SITE MAP
Home / About L.D.P.S & Services Offered / Learning Disabilities / Attention Deficit/Hyperactivity Disorder / The Learning Pyramid /
Articles, Papers & Information Sheets / Classes & Workshops / Related Links & Resources & References / Client Feedback
QUICK JUMPS ON THIS PAGE
What is Attention Deficit Hyperactivity Disorder? / Incidence / Diagnostic Criteria / A Reconceptualisation of ADHD /
Causes of ADHD / Implications / Management and Interventions / Conclusion / References


ADD & ADHD
- Attention Deficit Disorder &
Attention Deficit Hyperactivity Disorder
Attention Deficit Disorder (ADD) is a neurological disorder that affects children from the first months of their lives, through their school years, and into adolescence and adulthood. It may be accompanied with hyperactivity and is then known as Attention Deficit Hyperactivity Disorder (ADHD). The hallmarks of ADD are difficulties with attention, impulsivity and hyperactivity, which can be in varying proportions. Individuals with the disorder have difficulty paying attention, tend to act quickly without thinking things through, rarely learn from past mistakes and have trouble sitting still for lengthy periods.
Until recently, Attention Deficit Disorder was considered a disorder of childhood only. It is now recognised that up to 70 % of all children with ADD continue to exhibit symptoms of the disorder as adults. The condition does not always resolve in childhood as previously thought. When ADD persists into adulthood it is often associated with secondary problems such as anxiety, depression, gambling, drug and alcohol abuse. Management of the problem in childhood decreases the risk of these secondary problems occurring later in life.
The onset of symptoms must occur before the age of seven and persist for six months or longer. In other words, a child cannot suddenly develop ADD; rather the signs must have been present for a relatively long time. No two individuals with ADD present exactly the same profile i.e. a child may have poor concentration and be impulsive without being hyperactive. Since there is no "gold standard" for testing ADHD (the diagnosis made is a differential diagnosis and one of exclusion) it is necessary to pay careful attention to the developmental history of the child and to the family medical history. Recent technological advancements such as continuous performance tests (CTP’s) and the quantitative electroencephalograph (qEEG) are now being used as an adjunct to the behavioural descriptors of the DSM-IV and to select the most appropriate neurofeedback training protocols.
Incidence
ADHD and ADD is present in all populations with varying prevalence. The incidence of ADD is worldwide and figures vary because of differing criteria used for diagnosis and methods of evaluation. Research (1991) suggests that ADD affects 10-20% of the school-age population The ratio of males to females in the general population is 3:1; in clinical populations it varies from 6:1 to 9:1 due to a referral bias. The condition is often recognised later in life for girls. ADHD referrals contribute up to 30-40% of all clinic referrals. There is a greater prevalence in adopted and foster children due to the higher prenatal risk factors (addictions - nicotine, alcohol, illicit drugs, gambling & mental illness) associated with ADHD among those who give their children up for adoption or have their children removed from their homes. Worldwide the incidence is:
|
Australia |
3-5% |
China |
11% |
|
USA |
3-8% |
Italy |
12% |
|
Germany |
8% |
New Zealand |
13% |
|
United Kingdom |
10% |
Spain |
16% |
(Dr Anna Orgill 1995)
Research with twins in Australia (Levy and Hay 1995) indicates a 91% concordance of ADHD in monozygotic (identical) twins. Similar studies worldwide (Biederman et al 1992; Faraone et al 1993; Gillis 1992; Dykman & Ackerman 1991) also reflect the same ratio. Dizygotic twins have the same concordance as other siblings. The concordance for other siblings is between 30 and 40% depending on who you believe.
Diagnostic Criteria for ADHD in Children
* Often fidgets with hands or feet or squirms in seat (adolescents and adults may describe a feeling of restlessness)
* Has difficulty remaining seated when required to do so
* Is easily distracted by extraneous stimuli
* Has difficulty awaiting turn in games or group activities
* Often blurts out answers to questions before they have been completed
* Has difficulty following through on instructions from others e.g. fails to complete tasks
* Has difficulty sustaining attention in task or play activities
* Often shifts from one unfinished activity to another
* Has difficulty playing quietly
* Often talks excessively
* Often interrupts or intrudes on others eg. butts into other children's games or adult conversations
* Often loses/forgets things necessary for tasks or activities at home or at school (eg.toys, pencils, books, sports gear, assignments)
* Often engages in physically dangerous activities without considering possible consequences (not for the purpose of thrill seeking) eg. runs into the street without looking
Eight of the above must be present to make a diagnosis of ADD.
Suggested Criteria for ADHD in Adults
Hallowell & Ratey (1994) list a chronic disturbance in which at least 15 of the following are present:
1. A sense of underachievement , of not meeting one's goals (regardless of how much one has actually achieved).
2. Difficulty getting organised.
3. Chronic procrastination or trouble getting started.
4. Many projects going simultaneously; trouble with follow through.(A corollary to No.3).
5. Tendency to say what comes to mind without necessarily considering the timing or appropriateness of the remark.
6. A frequent search for high stimulation.
7. An intolerance of boredom. (A corollary to No.6).
8. Easy distractibility, trouble focusing attention, tendency to tune out or drift away in the middle of a page or a conversation, often coupled with the ability to hyperfocus at times.
9. Often creative, intuitive, highly intelligent.
10. Trouble in going through established channels, following "proper" procedure.
11. Impatient; low tolerance for frustration.
12. Impulsive, either verbally or in action, as in impulsive spending, changing plans, enacting new schemes or career plans etc.
13. Tendency to worry needlessly, endlessly; tendency to scan the horizon looking for something to worry about, alternating with inattention to or disregard for actual dangers.
14. Sense of insecurity (despite security, they their world could collapse).
15. Mood swings, emotional lability, especially when disengaged from a person or project.
16. Restlessness ("nervous energy"; pacing, drumming of fingers, shifting position while sitting, leaving a room or table frequently, feeling edgy while at rest.
17. Tendency towards addictive behaviour (caffeine, alcohol, cocaine, smoking, gambling, shopping, overeating, overwork).
18. Chronic problems with self esteem.
19. Inaccurate self-observation.
20. Family history of ADD or manic-depressive illness or depression or
substance abuse or other disorders of impulse control or mood.
 Childhood history of ADD (signs and symptoms must have been there even if it was not formally diagnosed).
Childhood history of ADD (signs and symptoms must have been there even if it was not formally diagnosed).
 Situation not explained by other medical or psychiatric condition.
Situation not explained by other medical or psychiatric condition.
The idea of Adult ADHD is new and somewhat controversial. Many adults only realise they have ADHD when they seek a diagnosis for their son or daughter. Up to 65% of children previously diagnosed with ADHD will continue manifesting symptoms of the disorder into adulthood. Furthermore, anti-social behaviour can be seen in 20%-45% of adults with ADHD, while 25% develop an anti-social personality (Barkley 1990). 12% may develop substance abuse (Gittelman et al 1985, Mannuzza et al 1993, Wender 1981). Anxiety and somatic disorders were reported in approximately 79% of ADHD children in adulthood. Additionally, interpersonal problems were reported by 75% and sexual adjustment problems in about 20% (Silver 1992, Weiss & Hetchman, 1986). Serfontein (1994) also suggested that up to 10% of the jail population are adult sufferers of ADHD.
By adulthood, the problems of academic underachievement noted in childhood will usually have become worse, with 30% failing to complete high school and only 5% going onto university compared to 41% of control study children (Barkley, 1990).
None of this is surprising if you remember that these adults have struggled, usually undiagnosed, with problems in many areas throughout their lives. Most notable in Adult ADHD are problems in the following areas: concentration, spelling, writing, reading, memory, organisation, restlessness, rigidity, relationships, and having a short fuse.
Reconceptualisation of ADHD
Mounting evidence is increasingly suggesting that it is the behavioural class of impulsivity and hyperactivity , or poor regulation and inhibition of responses, that underlines ADHD.
The primary symptoms of ADHD can be more heuristically conceptualised as deficits in the functional relationships between child behaviour and environmental events rather than as cognitive constructs or capacities. ADHD is therefore a problem with the stimulus control or regulation of behavioural responses, particularly in the area of behavioural. inhibition. Evidence suggests that deficits in behavioural regulation may stem from one or more of the following impairments:
(1) diminished sensitivity to behavioural consequences,
(2) diminished control of behaviour by partial schedules of consequences,
(3) poor rule-governed behaviour.
Which of these may be proved to be primarily involved in ADHD is not yet clear. However, there is little doubt that present conceptualisations of ADHD as a problem in attention or impulsivity are losing their explanatory and prescriptive value, and are likely to be replaced by theories founded on motivational deficits rather than attentional ones.
Barkley (1997) proposes that response inhibition is a fundamental attribute linked to the performance of other executive functions viz: prolongation, separation and regulation of affect, internalisation of language, reconstitution and motor control and fluency. Tlere are three types of response inhibition: (1) the ability to inhibit a prepotent response (urge to act) before it happens (2) the ability to stop an ongoing response (action) that is ineffective, maladaptive or detrimental and shift to another (can you stop it quickly?) (3) the ability to protect the delay in response from outside interference. Acts of self control occur in the brain between the time the event occurs and the time it takes to respond. During this time interval the brain regulates action. Response inhibition is thus the key to these executive functions.
Barkley's Reconceptualisation of ADHD (1999)

Thus the label Attention Deficit Disorder is a misnomer. Labelling it as such trivialises the magnitude of the expression of the response. Barkley and several Australian practitioners (Hutchins, Green, Chee, Nash,) describe the attention part of ADHD as referring to the allocation of mental resources i.e. the mismatch of demands and resources and the disorder occurs because of response disinhibition which creates secondary impairments in the executive functions which lead to deficient self-regulation as well as impairment in the organisation of behaviour over time which results in deficits in social/adaptive behaviour. Individuals with ADHD don't have a problem knowing what to do, they have difficulty doing what they know!
T'he clinical and legal implications of this reconceptualisation of ADHD are therefore enormous.
Causes
While researchers still disagree on the exact cause of ADHD/ADD (Weinberg & Brumback 1992), two things are certain. First, it is an hereditary condition. Second, the problems of ADHD result from a subtle difference in the fine tuning of the brain. Neurological immaturity, decreased activation of the brain's reward system, dysfunction of the reticular activating system, deficits in the motivational system and underarousal of the brain have all been proposed to explain ADHD symptoms (Wender 1971, Silver 1992, Barkley 1990). Only 3-5% of ADHD have a history of significant brain injury and such injuries are unlikely to account for the majority of children with this condition.
Heredity
Most children with ADHD seem to have a close relative with a similar problem. Often it is the father who found school years difficult or who underfunctioned academically for his abilities. Some ADHD adults have done very well in life but are still restless and inattentive, and fitted with a dangerously short fuse.
Additionally, ADHD and Learning Difficulties share the same genetic influence particularly in the areas of speech and reading (Levy & Hay 1995). Thus an ADHD child of a parent with both ADHD and LD usually inherits both the attentional and reading problems together.
Researchers now believe that a gene variation associated with AD/HD first appeared between 10,000 and 40,000 years ago and was probably a significant advantage to the early humans who had it. Specifically, DRD4 7R - is a gene associated with traits such as novelty-seeking, increased aggression and perseverance. According to Dr. Robert K Moyzis, in the January edition of the journal Proceedings of the National Academy of Sciences of The United States of America, possessors of these traits would have been more likely to survive the times.
This would seem to support Thom Hatmann's controversial hunter-gatherer theory of ADHD which he wrote in 1993. In light of these findings we will need to redress and reconceptualise our model of ADHD.
Perhaps our education ministers should be following the need of these children, and revisit the way our schools and classrooms are organised. "The Hunter School" in the United States follows a curriculum based upon instructional concepts created by Hartmann and others.
Neurological Function
At present the main research interest is in three areas: assessing frontal lobe function (the seat of executive control), studying the message transmitting brain chemicals (neurotransmitters), and investigating areas of under- and overfunction (SPECT scans). Since there are no significant lesions in ADHD/ADD, the use of EEG, CAT scans and MRI was ineffective since they only detect abnormalities in the superficial layers (cortex) and do not tap into the deeper parts of the brain.
In the late 1980's SPECT and PET scans looked at blood flow and glucose metabolism in different parts of the brain. Zametkin's 1990 study found that ADHD individuals metabolised glucose at rates 8% lower than the control group when performing continuous performance tests specifically designed to measure attention and vigilance to stimuli. This decrease in metabolic activity was most noticeable in the prefrontal and premotor regions of the brain. Additionally, decreased blood flow was indicated in the frontal lobes and the posterior periventricular region of the right hemisphere (Lou et al 1990). The caudate nuclei/striaturn were the most consistent areas of underfunctioning in ADHD individuals.
|
|
|
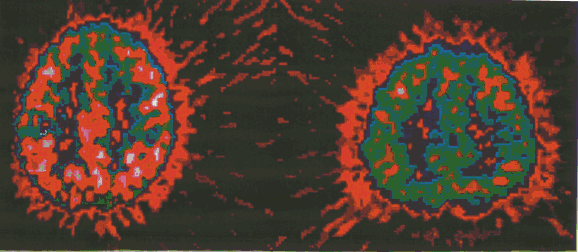
NON-ADHD ADULT |
ADHD ADULT |
|
ATTENTION DEFICIT-HYPERACTIVITY DISORDER (ADHD) IS REAL! |
(There is a difference between these two brains. Positron emission tomography (PET) studies show that the rate at which the brain uses gluclose its main energy source, is lower in subjects with ADHD as compared to normal subjects. Alan Zametkin M.D., and his team of researchers at the National Institute of Mental Health published their landmark findings in the New England Journal of Medicine in November, 1990).
The striatum, frontal lobes and posterior periventricular regions are known to underlie aspects of response inhibition, inattention and incentive learning or sensitivity to reinforcement. As well as having complex connections with each other, these three regions are richly interconnected with the sensory cortices. They act as a gate, allowing important information to register but filtering out the noise of interfering information which prevents us from focusing on relevant messages. Because these "filters" are underfunctioning in ADHD they are unable to gate the hundreds of unimportant stimuli that arrive every minute. This constant unchecked bombardment shows up on SPECT scans as increased blood flow in regions that receive sight and sound stimuli (Stuss & Benson 1986; Heilman et al 1990; Lou et al 1989; Zametkin & Rapoport 1986).
When Ritalin was administered to ADHD children, its effect showed up on SPECT scans as a redistribution of blood flow in the brain (Klorman 1991). It appeared to increase the level of function of the under-perfused regions of the striaturn, posterior periventricular region and to a lesser extent the frontal lobes. This normalisation allowed the clutter of irrelevant messages to be screened out, which could then be seen as a reduction in blood flow to the vision and hearing areas. This filtering of irrelevant distraction helps concentration.
Additionally, evidence suggests that there appears to be both a reduction and imbalance in noradrenaline and doparnine which regulate the electrical/chemical feedback loop that controls behaviour (Bowden et al 1988, Heilman 1991, Riccio 1993). It has been suggested that dopamine forms a pathway between the motor centre and the frontal regions of- the brain, and another pathway from the limbic centre to the frontal regions of the brain. Thus dopan-line may have a role in connecting motor activity, emotion, attention and impulse control since it runs through the regions of the brain that regulate those functions.
Furthermore, dopamine and noradrenaline may regulate the overall output of the cortex. Speculations as to the role of working memory in ADHD are interesting (Goldman-Rakic). Working memory controls our ability to review our past, evaluate the present situation, and plan for the future. Without working memory, the world would be perceived as a series of discontinued events (like a series of unrelated slides) rather than a sequence (like a movie). One of the most frustrating aspects about ADHD is the inability to profit from experience, to focus on consequences and to navigate through tasks and social situations by what one has learned previously. If working memory is expressed in the frontal areas of the brain, and if the frontal lobes under-function in ADHD can we conclude that ADHD individuals have impaired working memories? At this stage the answer is no. This is an avenue for future research as methods of investigation and measurement become more sophisticated.
The right hemisphere controls executive or decision making capacities, visual-spatial abilities and our ability to process many sources of stimuli simultaneously. This dysfunction could prevent one from grasping the "big picture" (never quite understanding other people, always getting lost, losing things).
Functional neuroimaging studies carried out on individuals with ADHD have shown abnormal functioning of the anterior cingulate cortex (ACC) during tasks of selective attention. In a recent fMRI study (2006) the effect of neurofeedback training on the neural substrates of selective attention in children with ADHD was investigated. Fifteen un-medicated ADHD children who had no other comorbidities (co-existing conditions) were randomly assigned to the neurofeedback training group (experimental group) and the other five children were assigned to the control group (no neurofeedback training). The children were scanned (fMRI) while they performed the Counting Stroop test. Prior to neurofeedback training activation was evident in the left superior parietal lobule in all the children. After neurofeedback training, only those in the experimental group showed significant activation of the right anterior cingulate cortex - the key neural substrate of selective attention. (Johanne Levesquea et al, Neuroscience Letters, Vol 394, Issue 3, 20 February 2006, p 216-221)
Comorbidities
Research has repeatedly shown that ADHD is often accompanied by other brain-related problems. Major depression, bipolar disorder (manic depression), anxiety disorders, oppositional defiant disorder (ODD), and Tourette’s Syndrome (tic disorder) are all found more commonly in both children and adults with ADHD (Biederman, 1993, Hornig 1998). Additionally, brain researchers are now beginning to explore the connection between addictions and ADHD (Willens et al 1997). Those with ADHD are also more likely to experience "reward deficiency syndrome" as their brains crave adequate levels of daily pleasure through simple daily activities. Thus those with ADHD are literally "sitting ducks for addictions" (M. Lyon , 2000).
 NOTE: Untreated ADHD or ADD can result in "self-medication"
NOTE: Untreated ADHD or ADD can result in "self-medication" 
click here>
SEE THE RELATIONSHIP BETWEEN MARIJUANA ABUSE AND ADHD<click here
click here>
ALCOHOL AND BRAIN SHRINKAGE <click here
Furthermore, significant working memory deficits are common in individuals with ADHD (Benazra 1988, Felton 1987, Douglas 1990). Working memory enables a person to organise and efficiently complete tasks that are in front of them. Without a normal working memory the person has a very poor sense of time. Learning difficulties (slow reading, slow speed of processing information, difficulty following directions, learning maths tables) often result from this deficit. Unexpectedly, this lack of working memory is accompanied with the ability to "hyper-focus" on things they are interested in to the exclusion of everything else and may in part explain the "absent-minded professor syndrome". This ability to hyper-focus is potentially one of the most positive traits that accompanies ADHD. Those who learn to harness and direct this dynamic trait in a positive way can learn to soar high above their apparent disabilities and end up being very productive citizens (many high profile businessman have developed this trait).
In addition to ADHD being a brain problem, a wide range of physical complaints have been observed in children and adults with ADHD. These include: recurrent headaches, muscle aches and pains, abdominal pain (bacterial infections, intestinal parasites, food allergies, neurotoxins [Needleman 1993, 1995, Minder 1994], environmental toxicity [Cooley 1998, Lundin 1999]), severe fatigue, allergic disorders (asthma, eczema), respiratory infections and ear infections (for every ear infection, it can take from six to eight weeks for normal hearing to be restored after the acute phase of the infection has passed. This means that if a child has say, 6 recurrent ear infections he/she will have lost 24-48 weeks of accurate language reception and storage). Furthermore, addictions are common in children and adults with ADHD. Allergic and respiratory symptoms become less frequent during adolescence and adulthood and physical symptoms become harder to define. However, many adults report a general feeling of malaise most of the time. Many adults eventually suffer from fibromyalgia (disabling condition of muscle pain and fatigue) or chronic fatigue syndrome (severe fatigue and numerous other conditions).
These conditions make the conventional (parent, teacher questionnaire and rating scales approach) to the diagnosis and drug oriented management of ADHD far more complicated than with ADHD alone. The drugs used potently increase or decrease the activity of very specific neurotransmitters which may result in the improvement of some symptoms and no improvement of others or to non-ADHD symptoms worsening (Tourette’s syndrome).
Implications
ADD can affect how a person functions at home, at school and socially.
At home..
These children demand a lot of attention, easily forget instructions, constantly lose belongings, are disorganised and always on the go. They are often poor eaters and sleepers. Allergies and sensitivities to light, touch and sound are also common. They have difficulty getting on with their siblings and peers, are easily frustrated, and resist changes in routine. Social skills training together with behaviour modification program and dietary intervention are effective strategies to improve harmony in family life.
At School...
Learning disabilities e.g. working memory and short-term memory deficits, co-ordination problems, messy handwriting, speech and language difficulties, reading & spelling problems, dyscalculia, visual and auditory processing deficits are often associated with children who have ADD. Short-term memory is crucial to a child's ability to learn and learning can occur without it. Auditory and visual processing problems reflecting immaturity in the Central Nervous System are common. Verbal information tends to "go in one ear and out the other" whilst inefficient visual processing results in copying errors and skipping endings/words during reading. Poor verbal and written expression is another manifestation of short-term memory deficits.
Furthermore, up to 60% of ADD children exhibit some dysfunction in early speech development. These include articulation problems, stuttering, poor construction of sentences (incorrect use of syntax & grammar- nouns, mixing tenses, adjectives, adverbs), and sequential difficulties within words and sentences e.g."psighetti" instead of "spaghetti" or "I ball catch" instead of "I catch the ball". While receptive language develops reasonably well, the child's expressive language skills are often delayed. Speech problems are evident in pre-school children whilst language disorders are more evident in primary aged children.
Co-ordination problems are also frequent in children with ADD. Numerous research studies indicate that those with ADHD, dyslexia and dyspraxia (motor planning problems) are deficient in essential fatty acids (EFA’s) (Stordy, 1990). Balancing, posture, throwing, kicking, catching balls, doing up shoelaces & buttons, drawing and handwriting and other eye-hand coordination skills are often poor. Supplementation of EFA’s and daily exercises to inhibit retained primitive reflexes is suggested in order to ameliorate these symptoms.
Since the child with ADD is unable to sustain attention long enough to retain auditory information and to process it sequentially, there are often large gaps in the acquisition of basic language skills. Effective and adequate remediation which address all of the above areas is vital for these children and may include sound therapy and craniosacral therapy to improve auditory processing disorders.
Socially...
Children with ADD are often socially immature. Lacking in pragmatic language skills they fail to read the cues of body language and thus making friends and developing satisfactory peer relationships is often difficult for them. Their low tolerance for frustration leads to temper tantrums or sulking. Inflexibility and inability to adjust to changes in the environment may be so pronounced that they are unable to make decisions and abide by them.
Self-esteem problems are both primary and secondary in children with ADD. They do not develop an appropriate self concept (because of brain dysfunction) and have difficulty relating to their family and peers. The lack of achievement in scholastic, sporting or social circles further exacerbates the primary problem, so that by adolescence they are at greater risk of being influenced by peer pressure. Being easily led and set up by their peer group, they are consequently more prone to find themselves in trouble. Feelings of inadequacy, anxiety and depression are therefore more common. As many as 30% will go on to develop Conduct Disorder or Oppositional Defiant Disorder.
ADHD as a Strength
The individual with ADD often possesses very positive and desirable qualities. However, these are often forgotten or overlooked as most of the attention is focused on the negative features of his behaviour and personality.
Some people with ADHD may appear blase, indifferent, self centred or even hostile when they are simply confused or unaware of what is going on around them . They may be angry or may withdraw, both responses causing interpersonal damage. Other ADHD individuals can be unusually empathic, intuitive, compassionate and creative. It is as if somewhere in that tangled brain circuitry there is a special capacity to see into people and situations. They can be loving and caring especially to younger children and animals. They can also be kind and generous in friendship.
ADD individuals may be very intelligent, talented and creative in the fields of writing, art and computers. Their energy, physical strength, athletic abilities, skills and playfulness enable them to become involved in many different pursuits which can result in excellent work in the areas of hobbies and sports. Lateral thinkers, sensitive and creative, they can also be competitive, vigorous and ambitious. These strengths could result in many great ideas as they use their inquisitive and inquiring mind.
This may explain why ADHD is common among people with Type A personalities working in high energy/stimulus fields such as the performing arts, selling, advertising, sports - any high pressure, high stimulus kind of work. These professions allow for the action-oriented, bottom- line individual who likes lots of projects running simultaneously as well as allowing the expression of passion, emotions, impulsivity and thrill seeking.
Furthermore, several elements of the ADHD mind favour creativity (Hallowell & Ratey 1994). A working definition of creativity is the tendency to see life's elements in new ways, to combine personal experiences into new forms, to give shape to new ideas. These elements include:
1. Having a greater tolerance for chaos than most. For all the problems it can pose, it can also assist the creative process. In bearing with the tension of the unfamiliar and unknown, one can enable something new to come into existence. The very uncertainty with which ADHD people react to most stimuli allows for the messages to metamorphose before they solidify in the mind. This tendency to get things confused- so often the bedevilment of the ADHD brain- can enhance creativity.
2. Impulsivity. It could be said that creativity is impulsivity gone right. Creative thoughts happen unscheduled. Ideas and thoughts appear out of nowhere, on the wings of impulse. Nowhere is where most ADHD people live all of the time.
3. Hyperfocus. This capacity is often overlooked. Attention deficit is a misnomer. The difficulty is one with attention inconsistency. A child can be absorbed for hours on a model airplane or an adult can be obsessed with the completion of a project.
4. "Hyper-reactivity of the ADHD mind" (Barkley). People with ADHD are always reacting, even when they look calm and sedate they are usually churning inside, moving this piece of data and putting the idea on the fire to burn. Such hyper-reactivity enhances creativity because it increases the collisions in the brain. Each collision has the potential to create new light, new matter. The trick for the ADHD person is to harness these processes productively. Some people spend a life time trying. They burst with creative energy but like a live wire without a socket to plug into, they dispel their energy unchallenged. The challenge is to manage them in positive ways, to encourage them to use their assets and strengths to their advantage, and to guide them to achieve their potential.
Management and Interventions
Given the variety and magnitude of possible behaviours it is inconceivable to prescribe a panacea for the management of ADHD. Each case presents its own problems and requires its own solutions. Depending on the severity of symptoms and complexity of the situation, the management may last from a few sessions to several years.
Stimulant medication was first used in the management of ADHD in 1937 and Ritalin has been used since 1957. Dextroamphetamine and Methylphenidate (Ritalin) are mainly used in the management of ADHD. These are effective in over 80% of ADD children in the short term. While they do not cure ADHD, they improve some of the symptoms and can sometimes make other symptoms worse (Williamson 1997). However, stimulant medications come with side effects, most notably, increased heart rate and blood pressure, myocardial infarction, stroke and sudden death in children and adults on these medications (Nissen, SE, NEJM April 2006). Ritalin has also been associated with chromosomal changes that increase the risk of cancer three fold (2005). Despite the use of these stimulants since 1950, "the long term benefits and risks of stimulant treatment are not known definitively" (Anders, T & Sharfstein, S (2006) NEJM, May 2006, p2296). Other non-stimulant drugs eg. Clonidine (Catapres), Imipramine (Tofranil), Desipramine (Pertofran) and Moclobernine (Aurorix) are either used alone or in combination with the stimulants.
"Long-term studies indicate that a multi-modal interventioanl approach is necessary to achieve significantly improved outcomes for ADHD children. These studies indicate that psychostimulants alone do not improve the outcomes for most ADHD children. The data suggests that there may be a serious underutilisation of other interventional modalities and that the medical community may not be meeting the needs of many ADHD children. More promising outcomes have been reported when multimodal approaches are used in the management of ADHD. However, data on physician prescribing practices imply that few pediatricians provide treatment other than phamacotherapy with psychstimulants." (http://www.brainwavescenter.com/library/dea/dea2b.htm)
ADHD and its comorbidities are lifelong disabilities and will require adequate and effective ongoing multi-modal management and support. The management of ADHD must target both the ADHD and the comorbidities. A biopsychosocial approach such as the functional medicine model provides maximum benefit and no harm. When the principles of functional medicine are properly applied a wide array of the above mentioned symptoms may all improve or completely resolve. Functional medicine seeks to correct and resolve the underlying factors that have led to the symptoms in the first place. As Michael Lyons puts it ….. "the most important key in the management of ADHD lies not in the masking of symptoms, but rather in systematically uncovering and treating the underlying medical problems which are the heart of the this disorder" (p 50, Healing the Hyperactive Brain).

Diagram from Healing the Hyperactive Brain - by Michael R. Lyon M.D.pp321 -Focused Publishing - 2000
Multi-modal intervention includes any one or a number of the following:
 Parent education & support
Parent education & support
 Dietary intervention (nutritional supplements)
Dietary intervention (nutritional supplements)
 Neurofeedback (EEG Biofeedback & FNS)
Neurofeedback (EEG Biofeedback & FNS)
 Biofeedback (Psychophysiology)
Biofeedback (Psychophysiology)
 Educational interventions for the remediation of literacy skills
Educational interventions for the remediation of literacy skills
 Behaviour modification
Behaviour modification
 Psychostimulant medication (for more information click here)
Psychostimulant medication (for more information click here)
 SAMONAS Sound Therapy
SAMONAS Sound Therapy
 Exercises for the inhibition of Primitive Reflexes
Exercises for the inhibition of Primitive Reflexes
 Bowen Therapy
Bowen Therapy
 CranioSacral Therapy
CranioSacral Therapy
 Relaxation training & hypnosis
Relaxation training & hypnosis
 Social skills training
Social skills training
 Energy Therapies (EFT, Reiki, Bach Flower essences, Aromatherapy)
Energy Therapies (EFT, Reiki, Bach Flower essences, Aromatherapy)
 Meditation / prayer
Meditation / prayer
 Stress management
Stress management
 Discovering & nurturing a talent
Discovering & nurturing a talent
Conclusion
ADHD is the most researched disorder of childhood- a plethora of studies exist. Yet it remains poorly understood by the general public and often unrecognised or misdiagnosed by health professionals. The most dangerous aspect of undiagnosed and untreated ADHD is the assault on self esteem because the talents these individuals have, are never recognised and used: they give up, feeling lost and stupid.
ADD comes in many shapes and sizes. In many people, especially adults, the symptoms are masked by more obvious problems eg, depression, gambling, drinking and the underlying ADHD is never detected, usually being dismissed as "that's just the way he is". There is also much variability within the domain of diagnosed ADHD. ADHD/ADD is a condition which is intrinsically disorderly! Many adults with the disorder are undiagnosed until one of their children is diagnosed.
Therefore, it is of great importance that the diagnosis be made as early as possible so as to minimise the damage to self esteem that usually occurs when these children are misunderstood and labelled, lazy, defiant, or bad. The life of such a child and his/her family is a life full of unnecessary struggles, accusation, guilt, recrimination underachievement and sadness. The sooner the diagnosis can be made the sooner this unnecessary pain can cease.
The longer the diagnoses of ADD is delayed, the greater the chance of secondary problems developing. These include: depression, boredom, frustration, fear of learning new things, impaired peer relationships, drug/alcohol abuse, stealing and violent behaviour due to mounting frustration. These secondary symptoms are the most difficult to treat. It is important to remember that the management of ADHD is 90% education.
ADD is almost never a one person problem. It affects entire families, whole classrooms, careers and society. These individuals need our empathy, our expertise and our love to educate and advocate on their behalf. It all depends on our attitude - do you see ADD as a hidden handicap or rather as undeveloped hidden talent? If you conceptualise it as the stuff of champions, the stamp of genius then work to shaping and directing that incredible creativity and energy.
Individuals with ADD need not be perpetual victims of their diagnoses. There are no magic cures for ADD. However, it can be managed. Success with the multi-modal therapies outlined suggests that there is a lot they can do to help themselves. It is vital to is to identify and remediate their needs, discover and nurture their talents, advocate on their behalf, give them strategies to cope with stress and above all preserve their dignity in the process. Persistence, effort and time, together with powerful multisensorial remedial tools and effective therapeutic approaches enable these children to break the cycle of failure and frustration whilst significantly improving their skills and self-esteem.
References
ADHD Conference: Across the Lifespan: Living Successfully with ADRD. Conference notes, University of NSW, September, 1995.
Ambrosini, P.J., Bianchi, M.D., Rabinovich, H., Elia, J.,(1993) "Anti-depressant managements in children and adolescents: 11. Anxiety, physical and behavioural disorders". Journal of the American Academy of Child and Adolescent Psychiatry. 32: 483-493,
American Psychiatric Association (1994): Diagnostic and Statistical Manual -IV.
Anders, T., Sharsfstein, S (2006): "ADHD Drugs and Cardiovascular Risk". NEJM vol 354 (21), May 25 p 2296-2298.
August, G.J.,Garfinkel, B.D.,(1989): "Behavioural and cognitive subtypes of ADHD". Journal of the American Academy of Child and Adolescent Psychiatry. 28:739-748.
Barkley, R.A. (1995): Attention Deficit Hyperactivity Disorder: Workshop Manual
Barkley, R.A. (1991): Attention Deficit Hyperactivity Disorder: A Clinical Workbook, The Guilford Press, New York.
Barkley, R.A., (1990):ADHD Adolescents: Family Conflicts and their Management. Grant from National Institute of Mental Health, MH41583.
Barkley, R.A. (1990): Attention Deficit Hyperactivity Disorder: A Handbook for Diagnosis an Management. The Guilford Press, New York.
Bellak, L., Black, R.B., (1992): "Attention deficit hyperactivity disorder in adults", Clinical Therapeutics, 14: 138-147.
Benezzra E, Douglas V, (1988): "Short-term serial recall in ADHD, normal and reading-disabled boys". Journal of Abnormal Child Psychology. Vol 37, 225-7.
Berry, C.A., Shaywitz, S. E., Shaywitz, B.A., (1985): " Girls with attention deficit disorder: A silent majority? A report on behavioural and cognitive characteristics". Pediatrics 76: 801-809.
Biederman, J., Newcorn, J., Sprich,S (1991): "Comorbidity of attention deficit hyperactivity disorder with conduct, depressive, anxiety and other disorders". American Journal of Psychiatry. 148:564-577.
Biederman, J., Faraone, S.V., Keenan, K. et al. (1992): "Further evidence for family- genetic risk factors in attention deficit hyperactivity disorder: Patterns of comorbidity in probands and relatives in psychiatrically and pediatrically preferred samples". Archives of General Psychiat . 49:728-738.
Biederman, J., Faraone, S.V., Mick, E. et al (1993): "Patterns of psychiatric comorbidity, cognition, and psychosocial functioning in adults with attention deficit hyperactivity disorder". American Journal of Psychiatry. Vol150, 1792-8.
Bowden, C.L., Deutsch,C.K., Swanson,J.M.,(1988): "Plasma dopamine-beta hydroxylase and platelet monoamine oxidase in attention deficit disorder and conduct disorder. Journal of the American Academy of Child and Adolescent PVchiat 27, 171-174.
Cantwell, D.P., Baker, L., (1992): "Attention deficit disorder with and without hyperactivity : A review and comparison of matched groups". Journal of the American Academy of Child and Adolescent Psychiatry. Vol 31, 432-438.
Cantwell, D.P., Baker, L.(1991): "Association between attention deficit-hyperactivity disorder and learning disorders", Journal of Learning Disabilities, Vol 24, No 2 88-94.
Cooley, J.D., Wong, W.C., Jumper, C.A., Straus, D.C. (1998): "Correlation between the presence of certain fungi and sick building syndrome". Occupational & Environmental Medicine. Vol 55, 579-84.
DuPaul,G,J.,(1990) Parent and teacher ratings of ADHD Symptoms: Psychometric properties in a community based sample, Manuscript submitted for publication, University of Massachusetts Medical Centre , Worcester.
Douglas V, Benezzra E, (1990): "Supraspan verbal memory in attention deficit disorder with hyperactivity, normal and reading-disabled boys". Journal of Abnormal Child Psychology. Vol 18, 617-38.
Felton R, Wood F, Brown I, Campbell S, Harter M, (1987): " Separate verbal memory and naming deficits in attention deficit disorder and reading disability". Brain & Language. Vol 31, 171-84.
Forness, S.R, Swanson, J.M, Cantwell,D.P., Guthrie, D., Sena, R. (1992), "Response to stimulant medication across six measures of school-related performance in children with ADHD and disruptive behaviour", Behavioural Disorders, Vol 18 No 1, 42-53.
Gillis, J.J., Gilger, J.W., Pennington, B.F., DeFries, J.C. (1992): "Attention deficit disorder in reading disabled twins: Evidence for a genetic aetiology". Journal of Abnormal Child Psycholo . 20:303-315.
Gittlemann, R., Mannuzza, S., Shenker, R., Bonagura, N. (1985): "Hyperactive boys almost grown up: Psychiatric status", Archives of General Psychiatry , 42: 937-947.
Haenlein, M., Caul, W.F., (1987) " Attention deficit disorder with hyperactivity: A specific hypothesis of reward dysfunction. Journal of the American Academy of Child and Adolescent Psychiatry. 26: 356362.s
Hallowell, E.M. & Ratey J.J. (1994): Driven to Distraction- Recognising and Coping with Attention Deficit Disorder from Childhood through Adulthood. Touchstone
Heilman, K.M., Voeller,K.K.S., Nadeau, S.E.(1991): " A possible pathophysiological substrate of attention deficit hyperactivity disorder. Journal of Child Neurology . 6: S76-S79.
Hinshaw,P. (1987): "On the distinction between attentional deficits/ hyperactivity and conduct problems/ aggression in child psychopathology", Psychological Bulletin, Vol 101, No 3, 443-463.
Hornig M, (1998): "Addressing comorbidity in adults with attention deficit hyperactivity disorder". Journal of Clinical Psychiatry. Vol 57, Sup 7:69-75.
Hynd, G.W., Lorys, A. R,. Semrud-Clikeman,M, et al (1991),: " Attention without hyperactivity: A distinct behavioural and neurocognitive syndrome". Journal of Child Neurology Vol 6, S35-S41
Kaplan, B.J., Polatajko, H.J., Wilson, B.N., Farris, P.D. (1993): "Re-examination of sensory integration management:-a combination of two efficacy studies", Journal of Learning Disabilities, 26: 342-347.
Klorman, R., (1991): " Cognitive event-related potentials in attention deficit disorder". Journal of Learning Disabilities. 24:130-140.
Lambert, N.M., (1988): " Adolescent outcomes for hyperactive children", American Psychologist, 43, 786-799
Levesquea, J; Beaauregarda, M, Mensoure, B. (2006): "Effect of neurofeedback training on the neural substrates of selective attention in children with attention-deficit hyperactivity disorder: A functional magnetic resonance imaging study". Neuroscience Letters, Vol 394, Issue 3, 20 February 2006, p 216-221)
Lou, H.C., Henriksen, L., Bruhn, P., et al, (1989): "Striatal dysfunction in attention deficit and hyperkinetic disorder:, Archives of Neurology, 46: 48-52.
Lou, H.C., Henriksen, L., Bruhn, P. (1990): "Focal cerebral dysfunction in developmental learning disabilities", Lancet, 335: 8-11.
Lundin L, (1999): Allergic and non-allergic students’ perceptions of the same high school environment". Indoor Air.
Vol 9, 92-102.
Lyon, M. (2000): "Healing the Hyperactive Brain" Focused Publishing.
Mannuzza, S, Klein, R.G., Bessler, A., et al (1993): "Adult outcome of hyperactive boys: Educational achievement, occupational rank and psychiatric status". Archives of General Psychiatry. 50: 656-676. York: Permagon Press.
Minder B, Das-Smaal E, Brand E, Orlebeke J, (1994): Exposure to lead and specific attentional problems in schoolchildren". Journal of Learning Disabilities. Vol 27, 393-9.
Nash, H (1994): Kids, Families and Chaos: Living with Attention Deficit Disorder. Ed Med Publishers
Needleman, H, (1993): "The current status of childhood low-level lead toxicity". Neurotoxicology. 14, 161-6.
Needleman, H, (1995): "Behavioural toxicology". Environmental Health Perspectives. 103, 77-9.
Nissen, S.E, (2006): "ADHD Drugs and cardiovascular risk" NEJM, Vol 354 (14), 6 April, p1445-1448.
Riccio, C.A., Hynd, G.W., Cohen, M.J., Gonzalez, J.J.(1993): "Neurological basis of attention deficit disorder", Exceptional Children, 118-122, October/November.
Rhue, Lyn & Kirsh (1994): Handbook of Clinical Hypnosis. APA Washington, DC.
Serfontein, G. (1994): ADD in Adults: Help for Adults who Suffer from Attention Deficit Disorder. Paramount Communications Company.
Serfontein, G. (1989): The Hidden Handicap: Dyslexia and Hyperactivity in Children. Bateman.
Shaywitz, B. A., Shaywitz, S. E., (1991):"Comorbidity : A critical issue in attention deficit disorder". Journal of Child Neurology. 6:sl3-s2O.
Silver, L.B. (1992): " Diagnosis of attention-deficit hyperactivity disorder in adult life". Child and Adolescent Psychiatric Clinics of North America. 1:325-334.
Stordy, J.B, (1990) : School of Biological Sciences. University of Surrey, Guildford GU2 SXM. UK
Wilens T, Biederman J, Mick E, Faraone S, Spencer T, (1997): "Attention deficit hyperactivity disorder (ADHD) is associated with early onset substance use disorders. Journal of Nervous and Mental Disorders. 185: 475-82.
Williamson S, Gossop M, Powis B, Griffiths P, Fountain J, Strang, J (1997): :Adverse effects of stimulant drugs in a community sample of drug users". Drug & Alcohol Dependence. 44: 87-94.
For appointments for assessment, please contact:-
Rosemary Boon
, Registered Psychologist
Learning Discoveries Psychological Services
P.O. Box 9047 Harris Park NSW 2150
Telephone: (02) 9637 9998
Facsimile: (02) 9637 8799
Email:
ldps@bigpond.net.au
ADHD LINKS:-
 Alternative Therapies for Children with Developmental Disorders: Written and overseen by Lewis Mehl-Madrona, M.D., Ph.D. Program Director, Continuum Center for Health and Healing, Beth Israel Hospital / Albert Einstein School of Medicine, this site is a wealth of information for parents and professionals alike.
Alternative Therapies for Children with Developmental Disorders: Written and overseen by Lewis Mehl-Madrona, M.D., Ph.D. Program Director, Continuum Center for Health and Healing, Beth Israel Hospital / Albert Einstein School of Medicine, this site is a wealth of information for parents and professionals alike.




