|

|
Learning Discoveries
Psychological Services
Rosemary Boon Registered Psychologist
M.A.(Psych), Grad. Dip. Ed. Studies (Sch.Counsel),
Grad. Dip. Ed., B.Sc., MAPS, AACNEM. |
|
Telephone and Facsimile:
Sydney (+61 2) 9727 5794 |
Email:
rboon@iprimus.com.au |
Address:
P.O. Box 7120
Bass Hill NSW 2197
Australia |

MAIN SITE MAP
Home / About L.D.P.S & Services Offered / Learning Disabilities / Attention Deficit/Hyperactivity Disorder / The Learning Pyramid /
Articles, Papers & Information Sheets / Classes & Workshops / Related Links & Resources & References / Client Feedback

Fibromyalgia
Fibromyalgia is a soft tissue musculoskeletal syndrome that in many respects is similar to Chronic Fatigue Syndrome (it differs from Chronic Fatigue Syndrome (CFS) in that the primary symptom of fatigue experienced by CFS patients tends to be replaced more with musculoskeletal pain in fibromyalgia patients). The American College of Rheumatology established diagnostic criteria which includes pain on both sides of the body, both above and below the waist, as well as in an axial distribution (cervical, thoracic, or lumbar spine or anterior chest); additionally there must be point tenderness in at least 11 of 18 specified sites.
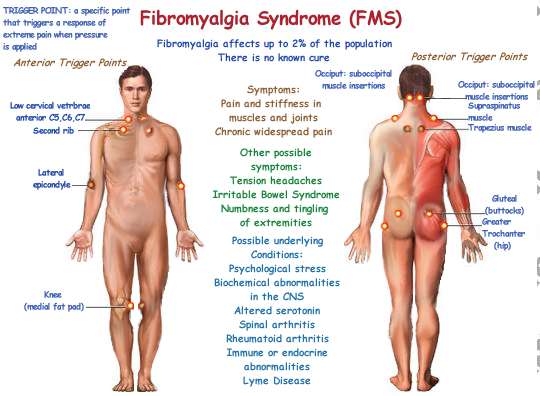
Stedman's Medical Dictionary describes the condition as "A syndrome of chronic pain of musculoskeletal origin but uncertain cause"
1..
As early nineteenth century, physicians documented a 'vague' condition involving fatigue, stiffness, aches, pains, and disturbed sleep patterns
2.. The origin of this condition, now known as fibromylagia syndrome (FMS), mystified physicians, and initially, some attributed the condition to the stress of modern life 2.. Others attributed it to inflammation in the body's fibrous tissue 3..
Currently, the aetiology of fibromyalgia syndrome (FMS) still remains elusive and FMS cannot be regarded as a distinctive disease, in the sense of having a uniform pathophysiogical basis, since its origin has yet to be determined 4., 8. . "While there is still not a majority of FMS researchers who support any one theory, significant progress is being made in identifying an aetiology"
5..
It has been noted that fibromyalgia often develops after physical trauma (i.e. an accident, injury or severe illness) which appears to act as a trigger in predisposed individuals. In 1997, a team of researchers found that there was a relationship between spinal injury and the onset of fibromyalgia. Cervical whiplash injuries tend to result in fibromyalgia-like symptoms around 90% of the time.
Symptoms of Fibromyalgia
A diagnosis of Fibromyalgia requires fulfillment of the following major criteria and 4 or more minor criteria:
MAJOR CRITERIA
 Cells: Fibromyalgia patients have been found to have a high incidence of damage to the Mitochondria of their Cells 6.
Cells: Fibromyalgia patients have been found to have a high incidence of damage to the Mitochondria of their Cells 6.
 Musculoskeletal System: The primary symptom of Fibromyalgia is chronic Musculoskeletal Pain characterized by
Musculoskeletal System: The primary symptom of Fibromyalgia is chronic Musculoskeletal Pain characterized by
Generalized pain or stiffness of at least 3 anatomic sites for at least 3 months; 11 or more typical, reproducible tender points (the American College of Rheumatology describes 18 points over Muscles and Tendons).
Exclusion of other ailments that can cause similar symptoms.
MINOR CRITERIA
 Digestive System: Irritable Bowel Syndrome
Digestive System: Irritable Bowel Syndrome
 Metabolism: Generalized Fatigue (similar to Chronic Fatigue Syndrome)
Metabolism: Generalized Fatigue (similar to Chronic Fatigue Syndrome)
 Musculoskeletal System: Joint and other soft tissues inflammation (swelling)
Musculoskeletal System: Joint and other soft tissues inflammation (swelling)
 Nervous System: Anxiety, Depression, Chronic Headache, Insomnia and other Sleep Disorders, Neurological and psychological ailments, Numbness, Variation in symptoms associated with activity, stress and weather changes, Vertigo
Nervous System: Anxiety, Depression, Chronic Headache, Insomnia and other Sleep Disorders, Neurological and psychological ailments, Numbness, Variation in symptoms associated with activity, stress and weather changes, Vertigo
Frequently misdiagnosed, fibromyalgia is often confused with myofascial pain syndrome, hypothyroidism, rheumatoid arthritis, chronic fatigue syndrome, and systemic lupus erythematosus, which often have comorbidity with fibromyalgia 7..
The pain of fibromyalgia usually consists of diffuse aching or burning sensations and is often accompanied by muscle spasm. It may be generalised or localised" 8. and can vary from day to day and can change location, becoming more severe in parts of the body that are used more often. In some people the pain can be intense enough to interfere with normal activities of daily living including occupational activities.
The fatigue associated with fibromyalgia may vary between individuals, ranging from a tired feeling to the exhaustion experienced with influenza. Symptoms are exacerbated by environmental and emotional stress, "or an uncaring physician who gives the patient the message that it is 'all in the head" 8..
The condition exists worldwide and whilst most prevalent in adult women, it can occur in children, the elderly and men.
Fibromyalgia may remit spontaneously with decreased exposure to stress, but can recur at frequent intervals or may become chronic 8..
Researchers have collected useful evidence during the past several decades to determine the link between FMS abnormalities in the hypothalamus (limbic system and other cerebral areas), the autonomic ("automatic" or self-controlling) nervous system and the HPA axis, which regulates production of certain hormones and the body’s response to stress as likely in the underlying cause of fibromyalgia 9..
The following are some significant points of investigation:
• psychological factors,
• deprivation of restorative sleep,
• local tissue factors,
• neurobiochemical abnormalities,
• physical trauma and viruses, and
• genetic factors.
Orthodox Medical Treatment of Fibromyalgia
Pharmaceutical Drugs
Ibuprofen is sometimes prescribed to persons afflicted with fibromyalgia (although clinical studies have shown that Ibuprofen is no more effective than placebo for the treatment of Fibromyalgia10.)
Amitryptyline is sometimes prescribed to persons afflicted with fibromyalgia (although amitryptyline provides some relief from fibromyalgia symptoms (NOT THEIR CAUSE), its long term use is discouraged due to the severe side effects associated with long term use of tricyclic Antidepressants).
Incapacitating areas of focal tenderness may be injected with a 1% lidocaine solution or in combination with hydrocortisone acetate suspension 8..
Alternative / Complementary Approaches to Fibromyalgia
The best practice management of FMS is one which incorporates a personalised approach, designed around the person's unique biochemistry and psycho-social profile. It needs to be comprehensive, ambulatory, patient motivated and determined upon patient involvement in order to better discover and resolve the individual underlying causes in each case, thus addressing the whole person, not just the physical symptoms.
Biofeedback techniques - utilises various physiological measures such as EEG, Heart Rate, RSA Breathing, Skin Conductance, Temperature, Electromyography - or muscle tension. These are then 'fed back' to the person via a computer monitor, the individual is guided into various states of relaxation and learns to monitor their own body tensions, rhythms and thoughts in order to promote balance in the autonomic nervous system (ANS) and musculoskeletal systems.
Nutrition and Diet - Supplemental and dietary nutritional education based around best support for the individual at the cellular level, - addressing such things as genetics, cell growth and function, allergic reactions, malabsorption and autotoxicity problems, bacterial overgrowth, as well as lifestyle and goal-setting coaching.
Aerobic Exercise - light aerobic exercise has been shown to be of benefit in reducing symptoms11..
At
Learning Discoveries, our approach looks at guiding and educating the person in their own innate capacities to attain balance and wellbeing in their lives.
Education is an essential component of our individualised programme that helps sufferers and their families develop appropriate expectations, understand limitations, and make informed treatment decisions. Education in the FMS dis-ease process and development of coping strategies, including stress recognition and management, sleep patterns, nutrition, energy conservation, pain management and cognitive–behavioral intervention programmes, and physical conditioning is valuable in teaching people how to help themselves.
After a thorough history and assessment which may include a QEEG, an individualised programme will be devised aimed at restoring balance in the autonomic nervous system, and outlook. These include a combination of any of the following:- education and counselling, diet and nutrition, biofeedback and/or neurofeedback training, heart rate variability training, breathwork, bodywork, meditation, postural and movement exercises.
Consultation is by appointment only, for further information please contact:-
Rosemary Boon
|
Telephone and Facsimile:
Sydney (+61 2) 9727 5794 |
Email:
rboon@iprimus.com.au |
Address:
P.O. Box 7120
Bass Hill NSW 2197
Australia |
HOME / BACK TO ABOUT LEARNING DISCOVERIES / BACK TO ARTICLES PAGE
References
:
1. Stedman's Medical Dictionary
2. ME Williamson, 1996, Fibromyalgia: A Comprehensive Approach, New York: Walker and Company.
3. S Krsnich–Shriwise, 1997, "Fibromyalgia Syndrome: An Overview," Physical Therapy 77, January.
4. Wolfe F., 1993, Fibromyalgia: on diagnosis and certainty. J Musculoskel Pain 1(3/4):17.
5. Bennett, RM, 1996 , "A New Era of Understanding," Paper presented at the Oregon National Convention on Fibromyalgia: A New Era of Understanding; Oregon Convention Center, Portland, Oregon; 6-8 September 1996
6. Bengtsson, A., et al., 1989, Mitochondria damage and Fibromyalgia, Journal of Rheumatology. 16(supplement 19):144-149.
7. DL Goldenberg, 1992, "Controversies in Fibromyalgia and Myofascial Pain Syndrome", in Evaluation and Treatment of Chronic Pain, Edited by GM Arnoff, Baltimore, Maryland: Williams & Wilkins.
8. The Merck Manual of Diagnosis and Therapy, 1999, Merck Research Laboratories, Whitehouse Station, New Jersey.
9. Gail K. Adler, MD, PhD, 1999, Harvard Medical School , American Journal of Medicine
10. Yunus, M. B., et al., 1989, Short term effects of Ibuprofen in primary fibromyalgia syndrome. Journal of Rheumatology. 16:527-532.
11. Gowans, SE., deHueck, A., Voss, S., et al., 2001, Effect of a randomized, controlled trial of exercise on mood and physical function in individuals with fibromyalgia. Arthritis Care Res, vol. 45, pp. 519--529
Fibromyalgia Links
:
HOME / BACK TO ABOUT LEARNING DISCOVERIES / BACK TO ARTICLES PAGE
BACK TO TOP OF PAGE

