|

|
Learning Discoveries
Psychological Services
Rosemary Boon Registered Psychologist
M.A.(Psych), Grad. Dip. Ed. Studies (Sch.Counsel),
Grad. Dip. Ed., B.Sc., MAPS, AACNEM. |
|
Telephone:
Sydney (+61 2) 9637 9998
Facsimile:
Sydney (+61 2) 9637 8799 |
Email:
ldps@bigpond.net.au |
Address:
P.O. Box 47
Harris Park NSW 2150
Australia |

MAIN SITE MAP
Home / About L.D.P.S & Services Offered / Learning Disabilities / Attention Deficit/Hyperactivity Disorder / The Learning Pyramid /
Articles, Papers & Information Sheets / Classes & Workshops / Related Links & Resources & References / Client Feedback
QUICK JUMPS ON THIS PAGE
About Anxiety / Categories / Symptoms / Origins / Causes of Anxiety Disorders / Children's Anxiety Disorders / Interventions /
Non-Drug Approaches To Anxiety / The Wholistic LDPS Approach / References

Anxiety
Fear is a basic human emotion that has been crucial for survival both as an individual and as a species. Anxiety is the normal reaction of an organism to a stressor which may be external - or internal. The anxiety reaction generally has two components - one physiological and the other psychological, and both are mediated largely by the adrenergic (adrenaline and norepinepherine - the key components in the "Fright, Flight or Fight" response) neurotransmitter system1..
"Anxiety disorders" is a term used to describe unbalance in an individual's feelings or 'states' of anxiety, that is, the levels of tension, nervousness, distress, or uncomfortable arousal which they perceive.

Edward Munch (1863-1944) vividly captured the terror often felt by persons with anxiety disorders in his painting "The Cry" shown above - (It is often translated as "The Scream").
DSM-IV (The Diagnostic and Statistical Manual published by the American Psychiatric Association) divides anxiety into five main categories: phobias, panic disorder, generalised anxiety disorder, stress disorders (including posttraumatic stress disorder, and acute stress disorder), and obsessive compulsive disorder. It further subdivides these into a series of sub-disorders:- anxiety disorder due to a medical condition, substance-induced anxiety disorder, and a special category of anxiety disorder not otherwise specified.
As in all things, scientists and researchers love to fragment things in order to better study them, and accordingly categorise them, however, it is usual to find that an anxiety disorder extends throughout the whole person, at many levels, so that many aspects of function will need to be addressed to restore balance.
Firstly, let us look at the five main categories of "anxiety":-
- Phobias
Persistent, irrational, and disruptive fears of a specific object, activity or type of situation. A fear can be classified as a phobia when it is substantially greater than what seems justified or when it has no basis in reality. Generally, people with phobias are aware of their fears being an irrational response, and wish to overcome them, but have a great dealing of difficulty in doing so. Phobias can be simple, social, or complex - as in agoraphobia.
a). Simple phobias encompass the irrational fears of objects (e.g., spiders, snakes, high places, 'the dark' etc.) Simple phobias are actually much less common than social or complex phobias.
b). Social phobias cover the extreme fear of being criticised by other people leading to avoidance of social interaction involving groups of people, meeting new people, speaking in public - or doing anything which might result in criticism of any kind.
c). Agoraphobia is the fear of open, or public places. It accounts for around 60% of all phobias. Statistically, the majority of agoraphobics are female, and the problem usually begins to develop in adolescence or early adulthood. In extreme cases of agoraphobia, the person is unable to leave their home.
- Panic Disorder
Panic disorder is characterised by brief, abrupt and unprovoked, recurrent episodes of intense and uncontrollable anxiety. The person feels suddenly apprehensive or terrified, and will usually experience difficulty with breathing, heart palpitations, dizziness, sweating and trembling. Often the person fears losing control of themselves. Or 'going crazy'.
- Generalised Anxiety Disorder
Called this because the cause is difficult for the person to identify and trace to any specific problem, hence 'general', persistent, and often debilitating high levels of anxiety that can last any length of time. Physical symptoms are often quite prominent in this form of anxiety.
- Stress Disorder
Presents as extreme reaction to a highly stressful event or situation, and is often linked to adjustment disorders or the mere fact of coping with change. Categories of stress disorder include posttraumatic stress disorder and acute stress disorder.
a). Posttraumatic stress disorder involves the reenactment of a traumatic event, including recurrent and painful memories, nightmares and flashbacks that are so strong that the person believes he or she is reliving the event. The event may be participation in war, or exposure to a disaster such as earthquake, flood or fire, or serious accident. Some victims are so plagued by these recurrences that they become apathetic and detached.
b). Acute stress disorder is characterised by acute, brief, reactions to stress, which directly follow a traumatic event and last fewer than four months. The sufferer may experience a sense of detachment from the physical and social worlds, including distortions or other changes of perception and disturbances of memory.
- Obsessive-Compulsive Disorder
OCD consists of unwarranted, persistent thoughts and irresistible impulses to perform a ritual to relieve those thoughts.
a). Obsession - unwanted images or impulses that the individual is unable to suppress. Obsessives are usually unhappy about the obsession and being unable to keep it out of their minds.
b). Compulsion - irresistible impulses to perform a relatively meaningless act repeatedly and in a specific manner. The sufferer does not cherish or enjoy the ritualistic behaviour and will often view the bahaviour as foreign to their personality. They are aware of the absurdity of their behaviour, but are nevertheless unable to stop it. Someone with a compulsion to wash their hands for example, may perform this ritual several hundred times a day - in addition to being time consuming, the compulsions are often costly to the person's wellbeing. Other common compulsions are counting things to make sure that they are all there, checking the placement of objects and checking that appliances are turned off.
Symptoms of Anxiety Disorders
Anxiety disorders create discordance in a person's wellbeing through mood, cognitive, somatic, and motor symptoms.
 Mood symptoms include the feelings of tension, apprehension and sometimes panic. Often those who feel the symptoms do not realise, or know exactly why they are feeling the way that they do. Sometimes this will lead to the person feeling depressed simply because they do not see any way to alleviate the symptoms.
Mood symptoms include the feelings of tension, apprehension and sometimes panic. Often those who feel the symptoms do not realise, or know exactly why they are feeling the way that they do. Sometimes this will lead to the person feeling depressed simply because they do not see any way to alleviate the symptoms.
 Cognitive symptoms may include a person's spending a lot of time trying to work out why a particular mood or symptom is occurring - when they are unable to identify the causes, frustration sets in. Often thinking about the problem only worsens it making it harder for the person to concentrate on other things.
Cognitive symptoms may include a person's spending a lot of time trying to work out why a particular mood or symptom is occurring - when they are unable to identify the causes, frustration sets in. Often thinking about the problem only worsens it making it harder for the person to concentrate on other things.
 Typical somatic (- i.e. bodily) symptoms include sweating, hyperventilation, high pulse or blood pressure, and muscle tension. All are characteristic of a high level of autonomic nervous system arousal. (See the article - Vital Energy and Wellness and the Relationship to Brain Function - which extensively covers aspects of autonomic nervous system function and dysfunction and the realtionship to homeostasis or 'good health').
Typical somatic (- i.e. bodily) symptoms include sweating, hyperventilation, high pulse or blood pressure, and muscle tension. All are characteristic of a high level of autonomic nervous system arousal. (See the article - Vital Energy and Wellness and the Relationship to Brain Function - which extensively covers aspects of autonomic nervous system function and dysfunction and the realtionship to homeostasis or 'good health').
Over time, these primary symptoms can result in secondary ones. For example, hyperventilation may lead to feelings of dizziness and breathlessness; muscle tension can result in headaches and/or muscle spasms; high blood pressure to stroke or cardiac problems. The expression of anxiety, somatically speaking, is greatly variable - for instance some people will complain of stomach aches, others of clammy palms or parasthesia (numbness, usually in the hands and feet) etc.
 Typical motor symptoms include restlessness, fidgeting, and various kinds of bodily movements that seem to have no particular purpose - (such as pacing, finger tapping, tics and the like). People are often unaware they are even doing these things.
Typical motor symptoms include restlessness, fidgeting, and various kinds of bodily movements that seem to have no particular purpose - (such as pacing, finger tapping, tics and the like). People are often unaware they are even doing these things.
There are three things that are generally considered in determining whether or not the anxiety a person is experiencing is the same that everyone occasionally experiences or is considered debilitating:-
1. Level of Anxiety- it is normal to feel a moderate level of anxiety in using an old run-down elevator, but it is another to be unable to use any elevator due to a fear that you will get stuck between floors or go crashing to the bottom of the elevator shaft. That is, the fear is the result of a non-real threat.
2. Justification for the Anxiety - we all feel somewhat anxious about sitting for an exam or undertaking a new experience, but it is not normal to feel that same level of anxiety when there are no precipitating events. That is, some form of intra-psychic conflict.
3. Consequences of the Anxiety - if the anxiety leads to maladaptive results such as losing your job because of an inability to leave home, then the consequences are sufficiently severe to lead to classification as having an "anxiety disorder". Here, the anxiety is not relieved by the amelioration of the objective situation.
Origins of the anxiety disorders
can be difficult to establish simply because of the high rate of comorbidity existent with the range of classified anxiety disorders, and there are many theoretical paradigms proposing alternative explanations, some of which are:-
Psychodynamic Explanations
Sigmund Freud (d.1939) divided anxiety into three types - objective anxiety, derived from threats from the exterior world - anxiety about such things as realistic financial problems, failure in work, or in personal relationships - corresponding to fear and which was not considered abnormal behaviour.
Moral anxiety - stemming from battles between the id and the superego and derived from fear of punishment by the superego and arising from conflict within the person over expressed impulses of the id.
Neurotic anxiety - derived from the person's fear that the superego (with the aid of the ego) will not be able to control the id, and that the person may not be able to avoid engaging in unacceptable behaviour. Freud believed that phobias occur when anxiety is focussed on one or more particular objects - the objects representing a conflict at a symbolic level. Freud believed that many anxieties originate in sexual conflicts. Neo-Freudians on the other hand recognised that other conflicts such as feelings of inferiority (Alfred Adler) or of trust (Erik Erikson), could also lead to anxiety.
Learning Theory Explanations
Classical conditioning is considered the main candidate for origins of anxiety in this school of thought. A fear response is paired with a stimulus that was previously neutral. According to classical learning theory, an unpleasant experience would have to happen to the person experiencing the anxiety for conditioning to take place. Contemporary theorists contend that it is possible to experience vicarious conditioning (Bandura & Rosenthal, 1966). Simply through observational learning we can be conditioned to experience anxiety. For example, we may have watched the devastating events of September 11, 2001 on television, and experienced anxiety and become phobic about the possibility of a similar attack occurring to us, solely through becoming vicariously conditioned. Operant conditioning also plays a part in the development of the anxiety disorders. For example, consider compulsive behaviour - Suppose that you have an irrational fear of bacteria, and washing your hands makes you feel safer at least temporarily. You are reinforced (rewarded) for the hand washing behaviour, but soon the fear returns. You wash your hands again. And perhaps again…………..
Cognitive Explanations
These focus on the kinds of thoughts that a person has in response to situations. For example, negative thoughts in association with some form of rejection become the normal 'thought pattern' - that is every time the person has to engage in an activity whereby they may relive the remotest possibility of rejection, thoughts of failure prevent the person engaging in that activity. These types of thoughts are then automatic thoughts or thought patterns which become a self-defeating cycle. (See Beck, Emery, & Greenburg 1985). Dr. Daniel Amen refers to these in his book "Change Your Brain - Change Your Life" as ANTS - Automatic Negative Thoughts.
Humanistic-Existential Explanations
According to the humanistic perspective, the person experiences a discrepancy between the perceived self and the idealised self, causing feelings of failure which in turn cause the anxiety. Rogers, in 1961, found that anxious people tend to indicate more of a discrepancy than do confident people, between the persons they believe they are and the persons they believe they should be. Fischetti, Curran & Wessberg, in a 1977 study, found that anxious people show lower social skills than do non-anxious people, which further reduces their confidence in themselves9..
Neuropsychophysiological Explanations
In this viewpoint, several explanations have been offered. Neurotransmitters (chemical messengers in the brain) may contribute to anxiety disorders. They include norepinephrine, dopamine, serotonin, and gamma-aminobutyric acid (GABA). For instance, abnormalities in GABA and serotonin may have a particular role in susceptibility to generalized anxiety disorder. Serotonin is also a major player in OCD.
Inhibitory neurons that serve to reduce neurological activity may function improperly in people with anxiety disorders. GABA (gamma-aminobutyric acid) may be low in the persons body and thus lower the activity of inhibitory neurons, causing an increase in brain activity and arousal level which can be experienced as a state of anxiety.
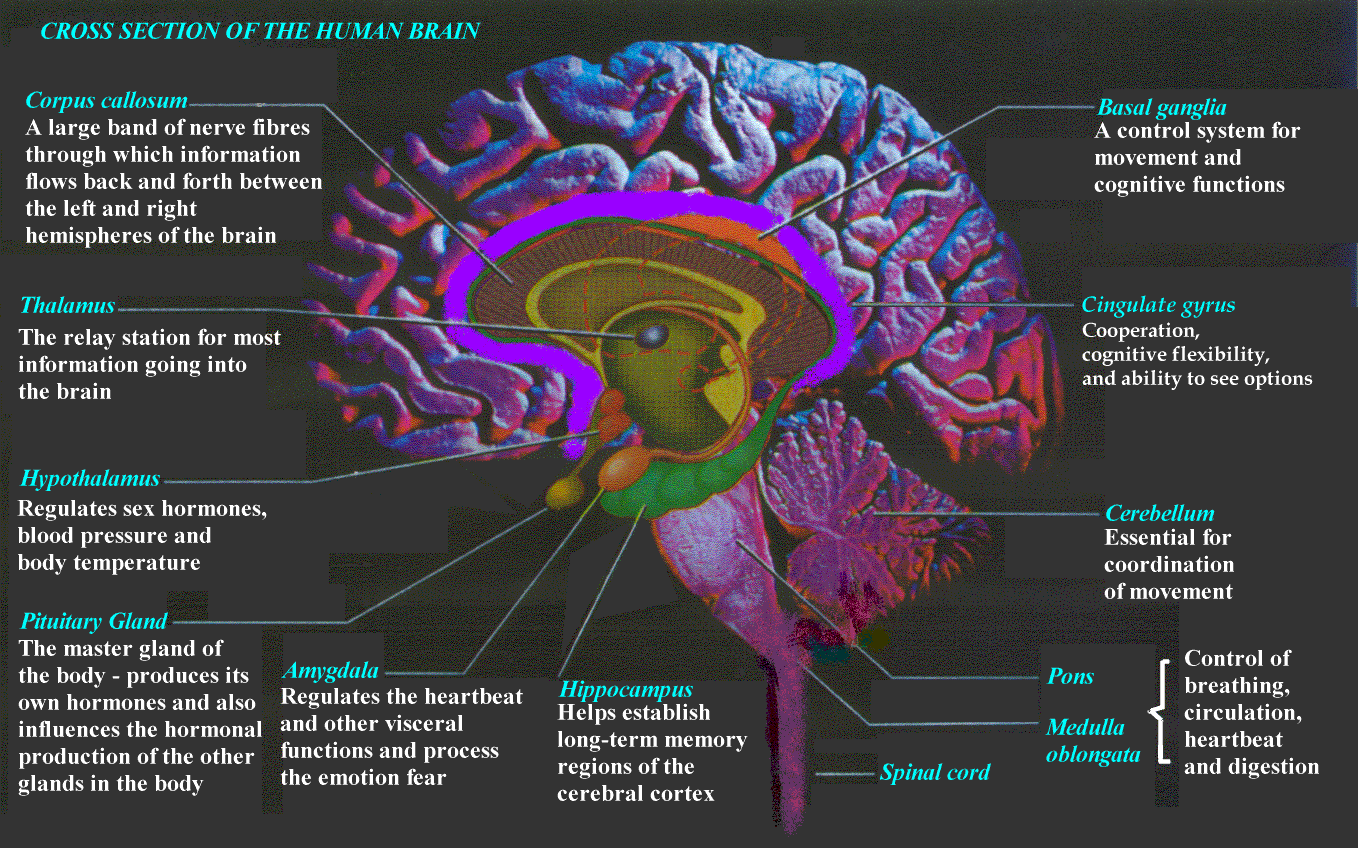
Scientists are now beginning to identify different areas and structures of the brain associated with anxiety responses using advanced imaging techniques. Recent studies by Dr. Daniel Amen using SPECT Scan imaging indicate that when the basal ganglia are over active, people are more likely to feel overwhelmed by stressful situations. (The basal ganglia is involved with integrating feelings, thoughts and movements and is responsible for setting the body's "idle speed" or anxiety level4.).
Abnormalities in a pathway of nerves, referred to as the basal-ganglia thalamocortical pathway, have been linked to OCD, attention deficit disorder, and Tourette's syndrome. The symptoms of the three disorders are similar and they often coexist.
One study using MRI imaging suggested that some children who develop OCD have a larger than average thalamus, which is a major messages center in the brain.
Some MRI scans have revealed over-activity in the locus coeruleus (a part of the brain important in triggering a response to danger) in people experiencing anxiety. A recent study using dual-probe microdialysis by Pudovkina, Kawahara, de Vries, and Westerink, confirms the release of noradrenaline in the locus coeruleus and prefrontal cortex5.. Further, this site in the brain is a centre of control for circadian rhythms as revealed in a study by Aston-Jones, G; Chen, Sheng; Zhu, Yan; Oshinsky, ML. In this study using trans-synaptic retrograde tracing it was found that a prominent indirect projection exists from the suprachiasmatic nucleus to the noradrenergic nucleus locus coeruleus (LC), a brain arousal system important in behavioral state regulation6..
Other studies have detected abnormalities in the amygdala, a part of the brain that regulates fear, memory, and emotion and coordinates them with heart rate, blood pressure, and other physical responses to stressful events.
An individual's environment, genetics, biochemistry, history - including familial history, and psychological profile all appear to contribute to the development of anxiety disorders. Most people with these disorders seem to have a biological vulnerability to stress, making them more susceptible to environmental stimuli than the 'normal' or average population.
All modes and schools of thought discussed so far have merit in the investigation of the causes of anxiety. When looked at in a wholistic manner, all of these factors come into play, - it is a whole person we are talking about, not just a coded classification of symptomatic anomalies.
 Genetic Factors and Family Dynamics.
Genetic Factors and Family Dynamics.
As you may have guessed, up to half of the people diagnosed with panic disorder have close relatives in whom the disorder is present, and about 20% of people with generalized anxiety have relatives with the same disorder. (About half of general anxiety disorder patients also have family members with panic disorder, and about 30% have relatives with simple phobias.) Obsessive-compulsive disorder is also strongly correlated to a family history of the disorder. Researchers are searching for specific genetic factors that might contribute to an inherited risk.
A 1999 study identified a possible genetic defect in OCD patients that affects serotonin, a neurotransmitter which appears to be important in anxiety disorders. Earlier, researchers identified a gene that produces lower amounts of serotonin in people who have personality traits that include anxiety, anger, hostility, impulsiveness, pessimism, and depression.
Other studies have identified a genetic defect that affects dopamine, another important neurotransmitter, which appears to cause a syndrome that includes migraine headaches, anxiety, and depression.
At an April 2001 meeting of the Human Genome Organization, Dr. Xavier Estevill, head of medical and molecular genetics at the Durani Rynals Hospital in Barcelona reported that a study he had conducted among a random sample of people with anxiety disorders, 97% had a duplication of genetic material on chromosome 15 -- compared with 7% in a comparison group of healthy people8..
Family influence upon anxiety is effected through both genetic and psychological factors. Many patients with anxiety disorders speak of parents who were at once overprotective and unaffectionate. One study suggested that stressful events, such as disagreements with parents, act upon internalized emotions in young adolescents. Eventually these feelings build up and produce full-blown anxiety or depressive disorders in young adulthood. Anxiety and depression are intimately linked.
Given that various findings are pointing toward a genetic predisposition as a primary cause of anxiety disorder, it should be remembered that not everyone who is predisposed toward anxiety will develop symptoms severe enough to seek help, however, there are triggers which may lead to anxiety disorders in susceptible individuals.
 Poor Breathing Patterns and Posture.
Poor Breathing Patterns and Posture.
Much research has been undertaken which suggests that in some people, rather than fear triggering a physical response, the opposite may occur. Some people with anxiety disorders have an abnormality in their breathing patterns that causes them to be very sensitive to carbon dioxide (CO2), resulting in hyperventilation (in which the breathing is rapid and the heart rate is fast). The condition may be aggravated in situations with high levels of CO2, (crowded or closed spaces, such as airplanes, elevators, etc.). In such circumstances, the person hyperventilates. Because such a response also occurs naturally during times of danger, the individual becomes frightened. Over time, a series of such responses creates a pattern (habit) of impaired breathing and panic that will evolve into a full-fledged anxiety disorder7..
 Traumatic Events
Traumatic Events
Traumatic events can trigger anxiety disorders, the most obvious being post-traumatic stress disorder, although there will usually need to be other psychological, genetic, or biochemical factors that make one susceptible to anxiety afterwards. Specific traumatic events in childhood, particularly those that threaten family integrity, such as spousal or child abuse, can lead to post-traumatic stress and other anxiety and emotional disorders. Some people may even have a biological propensity for specific fears, for instance of spiders or snakes, which can be triggered and perpetuated after a single first exposure.
 Other Factors
Other Factors
Anxiety can be a chronic symptom of other psychological or medical problems, such as depression, substance abuse, or thyroid dysfunction. A number of studies have reported a strong link between childhood rheumatic fever, which is caused by a streptococcal infection, and the development of tic-related disorders, including obsessive compulsive disorder and Tourette's syndrome. The effects of alcohol on the developing fetus appear to increase the risk for mental disorders as well as physical malformations.
 Other Medical Conditions.
Other Medical Conditions.
Anxiety-like symptoms are seen in many other medical problems, including epilepsy, hypoglycemia, recurrent pulmonary emboli, adrenal-gland tumors, and hyperthyroidism. Women can also experience intense anxiety attacks with hot flashes during menopause.
 Drug Side Effects. Many drugs, including some for high blood pressure, diabetes, and thyroid disorders, as well as some anxiety drugs can produce symptoms of anxiety. Withdrawal from certain drugs, often those used to treat sleep disorders or anxiety, can also precipitate anxiety reactions.
Drug Side Effects. Many drugs, including some for high blood pressure, diabetes, and thyroid disorders, as well as some anxiety drugs can produce symptoms of anxiety. Withdrawal from certain drugs, often those used to treat sleep disorders or anxiety, can also precipitate anxiety reactions.
 Overuse of Stimulants. Overuse of caffeine or abuse of amphetamines can cause symptoms resembling a panic attack.
Overuse of Stimulants. Overuse of caffeine or abuse of amphetamines can cause symptoms resembling a panic attack.
 Alcoholism and Substance Abuse.
Alcoholism and Substance Abuse.
People with anxiety disorders often drink alcohol or abuse drugs in order to conceal or ameliorate their symptoms, however, substance abuse and dependency can lead to anxiety. In addition, withdrawal from alcohol can produce physiologic symptoms similar to panic attacks. In such cases, clinicians often have difficulty determining whether alcoholism or anxiety is the primary disorder.
 Depression.
Depression.
Depression affects as many as 40% of patients with panic disorder. It is sometimes difficult to distinguish from anxiety disorders because depression is often accompanied by anxious feelings, agitation, insomnia, and problems with concentration. (Because of the confusion in making a diagnosis between the two disorders, the American Psychiatric Association is considering a new classification, mixed anxiety and depression.)
Children's Anxiety Disorders - are more than "simple fears"
"Children naturally have fears; it's part of growing up," says Deborah Beidel. "But when it stops being developmentally appropriate, then it's a problem. If fear is keeping a child from doing things that he should be doing--participating in school, playing, having friends, sleeping away from parents--then it's time to get help.10."
Children are most commonly affected by the following 5 anxiety disorders. R. Lindsey Bergman, PhD, associate director of the UCLA Child and Adolescent OCD and Anxiety Programme, defines them as problems when they disturb family life11.:
 Obsessive-Compulsive Disorder (OCD): Children with OCD require constant reassurance. They ask the same questions over and over, despite getting the same answer. They can also be quite rigid and unyielding about wanting things done in the same way. Whilst these behaviours can be seen as typical for a 4-year-old, they can be worrisome in a 9-year-old, and can become very troublesome if the behaviours are carried into adulthood..
Obsessive-Compulsive Disorder (OCD): Children with OCD require constant reassurance. They ask the same questions over and over, despite getting the same answer. They can also be quite rigid and unyielding about wanting things done in the same way. Whilst these behaviours can be seen as typical for a 4-year-old, they can be worrisome in a 9-year-old, and can become very troublesome if the behaviours are carried into adulthood..
 Separation Anxiety Disorder (SAD): Children with SAD are most commonly found sleeping in their parents' bed at night. What seems okay when the child is a toddler becomes a problem. If parents can't have privacy in their own room or can't go out of town and leave the child with relatives, experts say, then this is a problem that requires attention.
Separation Anxiety Disorder (SAD): Children with SAD are most commonly found sleeping in their parents' bed at night. What seems okay when the child is a toddler becomes a problem. If parents can't have privacy in their own room or can't go out of town and leave the child with relatives, experts say, then this is a problem that requires attention.
 Excessive Worry: A child with this problem is concerned with the "what-ifs" of life -- and worries over a variety of situations, many of them bizarre. This behaviour can be a result of the child's peronality style, as well as a disorder, but if it is interfering with normal development it will require attention.
Excessive Worry: A child with this problem is concerned with the "what-ifs" of life -- and worries over a variety of situations, many of them bizarre. This behaviour can be a result of the child's peronality style, as well as a disorder, but if it is interfering with normal development it will require attention.
 Social Phobia: Almost everyone is shy in some circumstances, but a child who has social phobia is so self-conscious and uncomfortable that they don't have friends and can't participate in school.
Social Phobia: Almost everyone is shy in some circumstances, but a child who has social phobia is so self-conscious and uncomfortable that they don't have friends and can't participate in school.
 Selective Mutism: Children with this problem do not to speak in certain situations despite speaking normally in others, exclusive of speech or language problems. In this instance - "It's hard to get treatment because schools often decide that the children are cognitively impaired and put them in special programs," Bergman says. "Getting them freed from that diagnosis is a problem itself." It is a sad fact that most school personnel simply do not have the expertise or experience to deal with a child having this disorder which is caused by anxiety and avoidance, and placement within "certain programmes" often only exacerbates the problem.
Selective Mutism: Children with this problem do not to speak in certain situations despite speaking normally in others, exclusive of speech or language problems. In this instance - "It's hard to get treatment because schools often decide that the children are cognitively impaired and put them in special programs," Bergman says. "Getting them freed from that diagnosis is a problem itself." It is a sad fact that most school personnel simply do not have the expertise or experience to deal with a child having this disorder which is caused by anxiety and avoidance, and placement within "certain programmes" often only exacerbates the problem.

Researchers seldom find a single factor that causes a psychological phenomenon. As each new insight into the workings of the human mind and body comes to light we obtain an increasingly detailed, more whole picture, enabling us to approach amelioration in a more wholistic manner, treating the whole person instead of just the symptom(s).
Interventions For The Anxiety Disorders
The best interventional option for you will depend on your specific diagnosis, symptoms, medical and familial history, and any co-existing physical or emotional problems.
 Screening Tests
Screening Tests
Although most family doctors can identify panic disorder, very few (10% only was cited in one study) recognise social phobias. Clinicians can use various tests to determine the causes, type, severity, and frequency of anxiety. Such tests include the Beck Anxiety Inventory, the Hamilton Anxiety Rating Scale, and the Anxiety Disorders Interview Schedule. As the tests are self administered, the problem with these tests lies in objectivity, yet they can be useful in a preliminary investigation and for monitoring the effectiveness of interventions.
A number of interventions exist including:
 Modern medicine
Modern medicine
 The current standard psychiatric/medical approach to most anxiety disorders is a combination of cognitive-behavioral therapy with medications, typically antidepressants, usually SSRIs or, less commonly, tricyclics. However, most general practitioners and family doctors will simply prescribe antidepressants as a first line intervention.
The current standard psychiatric/medical approach to most anxiety disorders is a combination of cognitive-behavioral therapy with medications, typically antidepressants, usually SSRIs or, less commonly, tricyclics. However, most general practitioners and family doctors will simply prescribe antidepressants as a first line intervention.
It is important to note that every drug manufactured, prescribed and ingested for amelioration of anxiety will create some side effect in the body which will ultimately affect the delicate balance of homeostasis required for optimal health.
In a recent study (2000) of panic disorder patients, CBT or a tricyclic antidepressant, either alone or in combination, were more effective than a placebo (a "dummy" pill). CBT, alone or with the tricyclic, was also very effective for long-term maintenance. After discontinuing treatment, however, CBT alone offered the best chance for a persistent response. Post-traumatic stress disorder (PTSD) is particularly difficult to treat, but SSRIs and specific behavioral approaches in the early stages of PTSD show promise according to current studies.
Drugs listed in the MIMS (An Australian Pharmaceutical Publication of approved drugs utilised by doctors) for anxiety are as follows:- Aldazine, Alepam, Amytal Sodium, Antenex, Ativan, Buspar, Chlorpromazine Injection BP, Deptran, Diazemuls, Diazepam Injection, Dothep, Ducene, Frisium, Kalma, Lesotan, Melleril, Murelax, Neulactil, Prothiden, Serepax, Sinquan, Stelazine, Surmontil, Valium, Xanax.
For Panic Disorders:- Aropax, Ducene, Kalma, Xanax and Zoloft.
Until recently, the anti-anxiety drugs known as benzodiazepines were the primary medications for anxiety. Increasingly, antidepressants, particularly the selective serotonin-reuptake inhibitors (SSRIs), are being used as the initial treatment. They are proving to be effective, physically nonaddictive, and to have relatively 'minor' side effects.
Many standard antidepressants require two to four weeks, and sometimes up to 12 weeks before they are fully effective.
People who take them may also experience a temporary period of increased anxiety.
Antidepressants
Selective Serotonin Reuptake Inhibitors (SSRIs).
Fluoxetine (Prozac), sertraline (Zoloft), paroxetine (Paxil), citalopram (Celexa), and fluvoxamine (Luvox) are antidepressant drugs known as selective serotonin reuptake inhibitors (SSRIs). They are prescribed by doctors and psychiatrists in a variety of anxiety disorders:
These drugs are the first-line of treatment for obsessive-compulsive disorder, and seem to reduce symptoms by 25% to 35% in about half of all patients. However, people with OCD and hoarding or compulsive behaviors may not respond as well to SSRIs as do those without these symptoms. In one study of children with OCD, Paxil therapy was associated with an apparent decrease in the size of the thalamus, a portion of the brain that is greatly involved with serotonin and may be enlarged in some people with OCD. SSRIs are also less effective in OCD patients with tics, for whom small doses of drugs known as neuroleptics may be helpful.
Zoloft and Luvox are used in treating patients with panic disorder. Some SSRIs appear to be of help to people with phobias, including agoraphobia and social phobias. However, relapse is common in social phobia patients even after prolonged treatment. Combining medications with cognitive-behavioral therapy can help prevent relapse.
Many SSRIs are prescribed for PTSD including fluvoxamine, sertraline, citalopram, and paroxetine.
According to the MIMS, the following side-effects have been reported with use of SSRIs:
Common Side Effects: Asthenia ("general weakness or debility"), headaches, malaise; agitation, anxiety, dizziness, insomnia, nervousness, somnolance, abdominal pain, anorexia, constipation, diarrhoea, dry mouth, dyspepsia, palpitatyions, tachycardia, sweating and terror.
Less common side effects of these drugs include: Ataxia (inability to coordinate voluntary muscle movement), confusion, extrapyramidal symptoms (motor symptoms external the motor system), hallucinations, hypotension, postural changes, Atralgia, myalgia, rashes, dermatitis, delayed ejaculation.
Rarer complications include: Convulsions, mania, liver dysfunction, photosensitivity, galactorrheoa.
Designer Antidepressants.
A number of newer antidepressants that target other neurotransmitters alone or in addition to serotonin include nefazodone (Serzone), venlafaxine (Effexor), and mirtazapine (Remeron).
- Venlafaxine is used for generalized anxiety disorder in other countries, but in Australia is widely used to treat major depression. The
'mechanism of its antidepressant action is thought to act' upon serotonin and noradrenaline reuptake as well as inhibiting dopamine reuptake. In some studies of patients with GAD, venlafaxine significantly reduced anxiety and improved overall well-being compared with placebo. As with the SSRIs, venlafaxine impairs sexual function. Of concern are reports of changes in blood pressure and heart conduction abnormalities, which may cause serious problems in elderly patients. Some patients report severe withdrawal symptoms, including dizziness and nausea. Other side effects listed in the MIMs as being observed in clinical trials of the drug were as follows:- Asthenia, chills, headaches, myalgia, agitation, anxiety, confusion, depersonalisation, depression, abnormal dreams, emotional lability, hypertonia, insomnia, decreased libido, nervousness, parasthesia, somnolence, abnormal thinking, tremor, dry mouth, urinary retention, rhinitis, sweating, pruritis, abnormality of visual accommodation, tinitus, abnormal vision, abnormal ejaculation/orgasm, impotence, - overdoses are frequent so dosage needs to be carefully monitored.
In one study, nefazodone was also effective in GAD patients (some of whom also had social phobias). The drug is more rapidly effective and has fewer distressing side effects, including sexual dysfunction, than SSRIs. It may cause an abrupt drop in blood pressure after standing up suddenly.
Combined Drug, and Non-Drug Treatment Options
Anxiety Disorder Benzodiazepines; buspirone; antidepressants, particularly extended release venlafaxine (Effexor) and some tricyclics Cognitive-behavioral, interpersonal therapy, stress management, biofeedback .
Panic Attacks SSRIs, benzodiazepines, tricyclics, MAO inhibitors, potentially, anticonvulsants Cognitive-behavioral therapy, including breathwork and nutrition.
Phobias Benzodiazepines, beta-blockers, SSRIs Cognitive-behavioral therapy (desensitization therapy), hypnosis.
Obsessive Compulsive Disorder SSRIs as first choice, except if tics are present (neuroleptics for tics), clomipramine (a tricyclic), MAO inhibitors for those who do not respond to other drugs Cognitive-behavioral therapy (Exposure and response prevention).
Post-traumatic Stress Disorder Antidepressants, particularly the SSRI sertraline, clonidine Cognitive-behavioral therapy (Group therapy).
Note: For anxiety disorders, the most common treatments prescribed are usually combinations of drugs and behavioral techniques
 Surgery
Surgery
At the top of the brain, in the middle of the frontal lobes is an area of the brain termed the "cingulate gyrus". It is the part of the brain which allows you to shift your attention from thing to thing, to move from idea to idea, to see the options in life. Feelings of safety and security have also been attributed to this part of the brain. The term that possibly best relates to this part of the brain is 'cognitive flexibility'.
Increased activity in the top, middle portions of the frontal lobes is frequently cited as a finding in obsessive-compulsive disorder, a condition where people become "stuck" on certain thoughts or behaviors. Aggressive people often become "stuck" on real or imagined injustices and think about them over and over. Oppositional, and addictive behaviours are also evident. Chronic pain, eating disorders and road rage appear to accompany cingulate dysfunction.
A surgical technique called cingulotomy involves interrupting the cingulate gyrus, a bundle of nerve fibers in the front of the brain. It is sometimes used as a last resort for patients with severe OCD. A recent variation of this procedure using magnetic resonance imaging (MRI) to guide the surgeon is resulting in long-term improvement in about one-quarter to one-third of OCD patients in whom it is performed. The procedure is hailed as generally safe with few serious complications and does not appear to affect intellect or memory12..
Given that the cingulate gyrus governs such things as:-
- The ability to shift attention
- Helping the mind move from idea to idea
- Allowing the mind to see options
- Cognitive flexibility (helps you go with the flow)
- Adaptability
- Ability to cooperate
One can only wonder at the long term implications of such a procedure and its effect on interrelations with others.
 Life Style Measures
Life Style Measures
A healthy, balanced lifestyle that includes exercise (movement - for the human body was designed to move), adequate rest, and proper nutrition can greatly help to reduce the impact of anxiety attacks. Rhythmic aerobic and yoga exercise programmes lasting for more than 15 weeks have been found to help reduce anxiety, probably due to the increased oxygenation of tissues - especially brain tissues, and production of endorphins. Strength, or resistance training alone does not seem to help anxiety.
As in all matters concerning health, personal responsibility for the maintenance of good health rests with the individual.
 Cognitive-Behavioral Therapy (CBT)
Cognitive-Behavioral Therapy (CBT)
The goal of cognitive-behavioral therapy (CBT) is to regain control of reactions to stress and stimuli, thus reducing the feeling of helplessness that often accompanies anxiety disorders. CBT works on the principle that the thoughts that produce and maintain anxiety can be recognized and altered using various techniques, thereby changing the behavioral response and eliminating the anxiety reaction.
A number of CBT approaches have been designed to treat both the general symptoms of anxiety and specific disorders. In one study of panic disorder patients, either CBT or a tricyclic antidepressant alone or in combination was as effective as short-term and maintenance therapy. After discontinuing treatment, however, CBT alone offered the best chance for a persistent response. Other studies have also reported similar benefits. CBT alone may be as effective as medications for children with OCD. Cognitive-behavioral therapy may even help people with post-traumatic stress disorder. CBT used in group therapy for children with PTSD may be especially helpful.
Treatments are equally effective in men and women. Anxiety disorders are chronic, however, and recurrence is common. Some studies indicate, in fact, that between 30% and 82% of people with panic disorder and phobias have a recurrence of attacks at an average of nine months even after successful short-term therapy. (Women are at much higher risk for recurrence of panic attacks than men.) Medications, then, are also generally recommended for most patients. There may be exceptions.
Basic Cognitive Therapy Techniques.
Treatment usually takes about 12 to 20 weeks. The essential goal of cognitive therapy is to understand the realities of an anxiety-provoking situation and to respond to reality with new actions based on reasonable expectations.
- First, the patient must learn how to recognize anxious reactions and thoughts as they occur. One way of accomplishing this is by keeping a daily diary that reports the occurrences of anxiety attacks and any thoughts and events associated with them. An OCD patient, for instance, may record repetitive thoughts.
- These entrenched and automatic reactions and thoughts must be challenged and understood. Again, using the OCD example, one approach is to record and play back the words of the repetitive thoughts, over exposing the patient to the thoughts and reducing their effect.
- Patients are usually given behavioral homework assignments to help them change their behavior. For example, a person with generalized social phobia may be asked to buy an item and then return it the next day, observing as he or she does so the unrealistic fears and thoughts triggered by such an event.!!
- As the patient continues with self-observation, he or she begins to perceive the false assumptions that underlie the anxiety. For example, OCD patients may learn to recognize that their heightened sense of responsibility for preventing harm in non-threatening situations is not necessary or even useful.
- At that point, the patient can begin substituting new ways of coping with the feared objects and situations.
 Systematic Desensitization.
Systematic Desensitization.
- Systematic desensitization is a specific technique that breaks the link between the anxiety-provoking stimulus and the anxiety response; this treatment requires the patient to gradually confront the object of fear and is especially effective for simple phobias, social phobias, agoraphobia, and post-traumatic stress syndrome.
There are three main elements to the process:
- Relaxation training.
- A list composed by the patient that prioritizes anxiety-inducing situations by degree of fear.
- The desensitization procedure itself, confronting each item on the list, starting with the least stressful.
 Exposure and Response Treatment.
Exposure and Response Treatment.
Exposure treatment purposefully generates anxiety by exposing the patient repeatedly to the feared object or situation, either literally or using imagination and visualization. It uses the most fearful stimulus first. (This differs from the desensitization process because it does not involve relaxation or a gradual approach to the source of anxiety.)
Exposure treatments are usually either known as flooding or graduated exposure:
- Flooding exposes the person to the anxiety-producing stimulus for as long as one to two hours.
- Graduated exposure gives the patient a greater degree of control over the length and frequency of exposures.
In both cases the patient experiences the anxiety over and over until the stimulating event eventually loses its effect. Combining exposure with standard cognitive therapy may be particularly beneficial. This approach has helped certain patients in most anxiety disorder categories. In one study, it even helped prevent PTSD from developing in motor-vehicle accident survivors with acute stress disorder. (The results of this study, however, are not necessarily applicable to other trauma sufferers, such as rape victims.)
 Modeling Treatment.
Modeling Treatment.
Phobias can often be treated successfully with modeling treatment:
- The therapy typically uses an actor who approaches an anxiety-producing object or engages in a fear-provoking activity that is similar to the patient's specific problem. Either a live or video-taped situation may be used, although the live model is considered to be more effective.
- The patient observes this event and tries to learn how to behave in a comparable manner.
Eventually, so-called "virtual reality" may prove to be a very useful modeling tool. This technology employs computer-generated images and special headgear to realistically simulate a natural environment and allow interaction with it. In one case, a psychologist used virtual reality to cure a woman of arachnophobia (fear of spiders). More research is needed.
 Relaxation Techniques and Breathing Retraining. As part of many of the CBT approaches, people are taught techniques to reduce the physical effects of anxiety. For example, many people with anxiety disorders experience hyperventilation, rapid, tense breathing that expels too much carbon dioxide, resulting in chest pain, dizziness, tingling of the mouth and fingers, muscle cramps, and even fainting. Hyperventilation is one of the primary physical manifestations of panic disorders. By practicing measured, controlled breathing at the onset of a panic attack, patients may be able to prevent full attacks. Relaxation methods, such as learning how to gradually relax all the muscles, may also be helpful.
Relaxation Techniques and Breathing Retraining. As part of many of the CBT approaches, people are taught techniques to reduce the physical effects of anxiety. For example, many people with anxiety disorders experience hyperventilation, rapid, tense breathing that expels too much carbon dioxide, resulting in chest pain, dizziness, tingling of the mouth and fingers, muscle cramps, and even fainting. Hyperventilation is one of the primary physical manifestations of panic disorders. By practicing measured, controlled breathing at the onset of a panic attack, patients may be able to prevent full attacks. Relaxation methods, such as learning how to gradually relax all the muscles, may also be helpful.
 Massage and Other Bodywork Therapies
Massage and Other Bodywork Therapies
Recent studies on massage have established that this therapy can lower an individual's blood pressure, make one feel more relaxed, relieve tension, soothe away headaches, relax tense muscles, or conversely, can be performed to make someone more alert. Massage can help preserve health, heal illness and relieve us from stiffness and pain. It provides us with a means to counteract stress and to deeply relax. Massage can be a journey of self-discovery, revealing how it feels to be more relaxed and in tune with ourselves, to experience the pleasure of a body that can breathe and be more in tune with itself.
Specific forms of bodywork including
Craniosacral Therapy and Bowen Therapy have also shown to be effective therapies in achieving autonomic nervous system balance.
 Biofeedback:- in its various forms, has a long history in relaxation training. Various physiological factors of body function and stresses in different parts of the body are fed back to the person in a manner that they can see and/or hear so that they can be taught to reverse them by training various parts of the body to relax.
Biofeedback:- in its various forms, has a long history in relaxation training. Various physiological factors of body function and stresses in different parts of the body are fed back to the person in a manner that they can see and/or hear so that they can be taught to reverse them by training various parts of the body to relax.
 EEG biofeedback (To read more, click on the blue link and use your browsers 'back-button' to return to this page).
EEG biofeedback (To read more, click on the blue link and use your browsers 'back-button' to return to this page).
Brainwave training is considered more global than other biofeedback modalities, as the brain governs the whole body. It is also a more automatic (easily done) form of biofeedback. Here the body and mind are guided into a profoundly relaxed alpha state enabling normalisation of autonomic nervous system activity and enhancing its inherent adaptability.
 Heart Rate Variability (To read more, click on the blue link and use your browsers 'back-button' to return to this page).
Heart Rate Variability (To read more, click on the blue link and use your browsers 'back-button' to return to this page).
Respiration and heart rate are intimately tied, so it is easy to see the implications of heart rate variability training in managing anxiety levels.
 EMG
EMG
Electromyography (EMG) was created by John Basmajian and measures the electrical potential of muscles. Anxious people generally hold tension in certain muscles. Tense muscles have a higher electrical potential. Here the primary targets are the frontalis (the forehead) as when people concentrate or worry, the will generally frown, or tense these muscles; and the muscles of the temporo-mandibular joint as people will also clench their jaw. Both of these actions will create the common 'tension headache'.
 Other Forms of Psychotherapy
Other Forms of Psychotherapy
Other forms of psychotherapy, commonly called "talk" therapies, deal more with childhood roots of anxiety and usually, although not always, require longer treatments. They include interpersonal therapy, supportive psychotherapy, attention intervention, and psychoanalysis. All work is done during the sessions. Some experts believe that such therapies might be more useful for generalized anxiety, which may require more sustained work to process and recover from early traumas and fears.
 Diet and Nutrition
Diet and Nutrition
Clinical anxiety may be associated with an elevated blood lactate level and an increased lactate to pyruvate ratio. 93% of those with neuroses compared to 20% of normals develop a panic attack following a lactate infusion 13. Furthermore, in schozophrenics, anxiety has been shown to correlate with lactate levels and with the lactate/pyruvate ratio 14. . Since alcohol increases the lactate/pyruvate ratio, it needs to be avoided. Avoidance of caffeine is also recommended particularly for those with generalised anxiety disorder and panic disorder since caffeine impacts serum epinephrine and norepinephrine concentrations. Sugar is also to be avoided as glucose can produce panic attacks in susceptible individuals by increasing the lactate/pyruvate ratio. Vitamin and mineral deficiencies also need to be corrected. Of concern are the B group vitamins (niacin, thiamine, B6 (impairs the conversion of tryptophan to serotonin), B12) Vit C, and Vit E). Calcium, magnesium, phosphorus, potassium and selenium deficiencies all increase nervousness, anxiety and increase the lactate/pyruvate ratio14.. Inositol (isomer of glucose) supplementation has been shown to be effective in agoraphobia and panic disorder with the EEG of these individuals resembling that of imipramine15.. Furthermore, essential fatty acid supplementation has also been found useful in some cases of anxiety. L-5 Hydroxytryptophan supplementation has been shown to cause a moderate reduction in anxiety (agarophobia and panic disorder) because it is the immediate precursor of the neurotransmitter serotonin16. . Other related nutritional factors in anxiety are food allergies/sensitivities and reactive hypoglycemia 16.-17.. The hypoglycemic connection was found through an informal study of 300 patients after undertaking a six-hour glucose tolerance test where it was found that blood glucose had dropped by 20% of their fasting level. Physiological and especially the neurological symptoms of anxiety were common. Previous treatments with tranquillisers, sedatives and or electro-convulsive therapy had proved ineffective. 85% responded favourably to a high protein, low carbohydrate, caffeine-free diet 18..
The Wholistic Approach at LDPS
At Learning Discoveries, our approach looks at guiding and educating the person in their own innate capacities to attain balance and wellbeing in their lives.
After a thorough history and psychometric assessment including a QEEG, an individualised programme will be devised aimed at restoring balance in the autonomic nervous system, and outlook. These include a combination of any of the following:- education and counselling, diet and nutrition, breathwork, biofeedbackand/or neurofeedback training, heart rate variability training, meditation and movement exercises.
Consultation is by appointment only, for further information please contact:-
Rosemary Boon
|
Telephone:
Sydney (+61 2) 9637 9998
Facsimile:
Sydney (+61 2) 9637 8799 |
Email:
ldps@bigpond.net.au |
Address:
P.O. Box 47
Harris Park NSW 2150
Australia |
References:
1.
Crow, S. F., 1998, Neuropsychological Effects of The Psychiatric Disorders, Harwood Academic Publishers, Melbourne, Australia.
2. Sternberg, R.J., 1995, In Search of The Human Mind, Harcort Brace & Company, Orlando, FL.
3. American Psychiatric Association, 1994, Diagnostic Criteria From DSM-IVÔ , American Psychiatric Association, Washington, DC.
4. Amen, D.G., 1998, Change Your Brain Change Your Life, Three Rivers Press, New York
5. Brain Research [Brain Res.], 2001, The release of noradrenaline in the locus coeruleus and prefrontal
cortex studied with dual-probe microdialysis, vol. 906, no. 1-2, pp. 38-45.
6. Nature Neuroscience [Nat. Neurosci.], Jul 2001, A neural circuit for circadian regulation of arousal, vol. 4, no. 7, pp. 732-738.
7. Han, J.N., Stegen, K. De Valck, C., Clement, J. & Van de Woestijne, K.P. (1996). Influence of breathing therapy on complaints, anxiety and breathing patterns in patients with hyperventilation syndrome and anxiety disorders. Journal of Psychosomatic Research. 41(5), 481-493
8. EMMA ROSS, Associated Press Medical Writer - Sun April 22, 2001 -Preliminary research suggests an unusual genetic abnormality may be linked to panic attacks and phobias. - EDINBURGH, Scotland (AP) --
9. Fschetti, M., Curran, S.P., and Wessberg, H.W., (1977) Sense of Timing. Behaviour Mondification, 1, 179-194.
10. Beidel, Deborah C.; Turner, Samuel M.; Taylor-Ferreira, Jill C. Behavior Modification. (1999 Oct) Vol 23(4) 630-646.
11. Piacentini, J., and Bergman, R.L., 2001, Developmental Issues in Cognitive Therapy for Childhood Anxiety Disorders, Journal of Cognitive Psychotherapy:, Volume 15, Number 3
12. Cosgrove, G.R., 1987, Surgical intervention to treat a psychiatric illness, Biological Psychiatry; 22:807-819.
13. Pitts, F.N., McClure, J.N. (1967): "Lactate metabolism in anxiety neurosis". New England Journal of Medicine, 277: 1329-36.
14. Werbach, M. R., (1999), Nutritional Influences on Mental Illness, (p70-82). Third Line Press Inc., Tarzana, CA
15. Benjamin, J., Levine, J., Fux, M., et al. (1995): "Double-blind, placebo-controlled, crossover trial of inositol treatment for panic disorder". American Journal of Psychiatry. 152 (7): 1084-1086.
16. Werbach, M. R., (1999), Textbook of Nutritional Medicine, (p110-115). Third Line Press Inc., Tarzana, CA
17. King, D.S. (1981): "Can allergic exposure provoke psychological symptoms? A double-blind test." Biological Psychiatry. 16 (1):3-19.
18. Salzer, H.M. (1966): "Relative Hypoglycemia as a Cause of Neuropsychiatric Illness". Journal of the National Medical Association 58 (1): 12-17.
Wilson, P., (1995), Instant Calm, Penguin Books Australia Ltd, Ringwood, Victoria.
DSM-IV is a coded reference manual published by the American Psychiatric Association to provide clear descriptions of diagnostic categories in order to enable clinicians and investigators to diagnose, communicate about, study, and treat people with various mental disorders. To view the DSM-IV criteria and revisions online please go to BraveNet
Ò Clinical Capsules at http://www.behavenet.com/capsules/index.htm. Use your browsers back button to return to Learning Discoveries, or better still, why not bookmark this site and add to your favourites?
Most of the above books are available through your local library or may be purchased on-line at


Rosemary Boon

L
EARNING DISCOVERIES
PSYCHOLOGICAL SERVICES
Telephone:
Sydney +61 2 9637 9998
Facsimile:
Sydney +61 2 9637 8799
Email:
ldps@bigpond.net.au
Address:
P.O. Box 47
Harris Park NSW 2150
Australia







