( This page is for patient information only and does not have any before and after pictures, testimonials or other advertisement & promotional material unlike other web sites )
Gall bladder stones are very common in developed countries and most developing countries including India and their prevalence increases appreciably with age; it is also determined by sex, body weight, and race. Fortunately, on most occasions, a gall stone does not cause severe symptoms such as pain and jaundice. They are best detected by ultrasound. Troublesome gall stones are generally treated by cholecystectomy (gall bladder surgery involving its removal along with the stones), and most of these procedures are carried out by laparoscopy. Medical terms used for gall bladder stone disease are cholelithiasis, chronic cholecystitis, acute cholecystitis, choledocholithiasis etc.
Gallbladder ?
Why we have a gall bladder at all is something of a mystery. Many animals such as horses, pigeons, and rats manage quite well without one. The gall bladder functions as an optional store for the bile secreted by the liver. Bile acids are important in making the fats in the intestine soluble before their digestion and absorption. The gall bladder contracts to eject high concentrations of bile into the intestine when a fatty meal is consumed but it does the same thing when any other sort of meal is taken or even when water is drunk. The gall bladder is clearly not essential to human digestion since patients who have had a cholecystectomy have no problems in this regard. In fact, sometimes it seems as if its main role is to keep doctors busy!!
In addition to bile acids, the liver secretes cholesterol and bilirubin into the bile, and herein lies the main problem. Cholesterol is not always in stable solution, even in perfectly healthy people, and can crystallize to form stones. In addition, the soluble conjugated bilirubin may be converted to free bilirubin, which then precipitates. The bile in the gall bladder is therefore an unstable concentrated "soup of chemical problems."
It is the presence of stones in the gall bladder that explains almost all of the ills inflicted by this organ. The process of stone formation is thought to be the result of a triple defect:
- Patients with gall stones have even more unstable bile than the rest of us
- They have more sluggish activity of the gall bladder, which allows crystals to grow into large stones
- They are also more prone to nucleate crystals in the first place, thereby initiating the process.
The major component of gall stones is cholesterol, which the liver clears from the body via the biliary tract and intestine, but bilirubin pigment on its own can form stones, and calcium salts also join in the process to a varying degree.
Who gets Gall Bladder disease ?

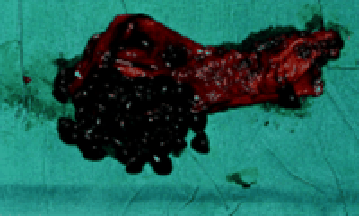 The picture on left is ultrasound showing stones and on right
the same gall bladder opened up to show the stones.
The picture on left is ultrasound showing stones and on right
the same gall bladder opened up to show the stones.
The prevalence of gall stones in the population can be measured conveniently by ultrasonography, and the prevalence of gallbladder disease is taken as the sum of people with gall stones and those who have had a cholecystectomy.
Gallstone disease has become more common in the west in the second half of the 20th century. This is partly because of the ageing population, but probably for other reasons too, such as increasing obesity in the population (figure). Doctors who believe that gall stones are a disease of middle aged women are mistaken.
 In India too the incidence is rising rapidly.
At Apollo Hospital, New Delhi, the author did a study on urban affluent people (
see adjoining graph) coming to the hospital for a routine health check and found
that 18 percent of females and 9 percent of males suffered from gall stones (
Over all incidence of 12% ). This is higher than the average incidence in US and
Western Europe of 8%. In New Delhi hospitals, a total of approximately 100 operations are done every day for this ailment.
In India too the incidence is rising rapidly.
At Apollo Hospital, New Delhi, the author did a study on urban affluent people (
see adjoining graph) coming to the hospital for a routine health check and found
that 18 percent of females and 9 percent of males suffered from gall stones (
Over all incidence of 12% ). This is higher than the average incidence in US and
Western Europe of 8%. In New Delhi hospitals, a total of approximately 100 operations are done every day for this ailment.
Though no definite theory is there to explain this phenomenon, the most accepted hypothesis is the changing dietary habits. Genetically, the Indian body for centuries, is used to a low calorie and less refined diet. The incidence appears to be higher amongst population where there has been a dramatic change in life style in one generation. People moving from rural to urban areas far from their origin also seem to be more susceptible. Although no gene has been identified, the disease does seem to run in families.
- Pregnancy increases the risk of gall stones, but the oral contraceptive pill does not. Although there is evidence that the high doses of oestrogens found in hormone replacement therapy may cause stones, we do not yet have definite proof that this is the case.
- There is general agreement that obesity causes stones, but even more so is the rapid weight reduction caused by a stringent diet or bariatric surgery.
- No particular food has been incriminated in the formation of stones. Nevertheless, vegetarians have fewer stones.
- It has also been proposed that moderate quantities of exercise, aspirin, and non-steroidal anti-inflammatory drugs are protective.
There is an international league table of gallstone prevalence. The United States and Western Europe lead the table while African countries are at the bottom. Gallstone disease tends to be a disease of more affluent societies, but there are clearly racial differences. However, the prevalence of gallstone disease in India has increased from a low level as a result of westernization of life style, suggesting that environmental factors are important. It is much more common in North India as compared to the rest of the country.
Various other problems can lead to gall stones.
- These include break down of blood seen in patients with childhood anemias (which causes an increased number of both pigment and cholesterol stones),
- diabetes, high cholesterol
- after stomach surgery
- some drugs and medicines, which reduces gallbladder motility and increases cholesterol saturation of bile.
Natural History of Gall Stones
If we take 100 patients of gall stones who do not have any trouble from them, and follow them up, 2 patients will develop trouble every year. This means there can be patients who would be trouble free even after 40-50 years. Unfortunately it is not possible to predict who will develop trouble and who will not. For these patients it is advisable to wait for pain and trouble from the gall stones before they go in for surgery.
However if we take 100 patients who have trouble from their gall stones, then 30 patients will develop complications every year. Treatment of complications is associated with a high risk and other problems during and after surgery. For these patients it is advisable to go in for surgery as soon as they develop pain and trouble from the stones and not wait for complications to set in.
Role of the doctors and specialists
The problem is to identify which patients belong to the first category and which patients belong to the second category. Here lies the duty of the doctor to identify and correctly advise. In case of doubt, the patients should be referred to specialists who deal with gall bladder problems and seek their advice. Unfortunately, even amongst the doctor community, there is not always consensus on who needs surgery and who does not.
Unfortunately, many patients undergo unnecessary surgery when they do not need it and their symptoms are totally unrelated to the gall stones which is just an incidental finding on ultrasound.
It is not necessary that all patients with gall stones should undergo surgery and only those with symptoms should be offered surgery as they are at risk for complications. The specialist has to identify the symptoms and then explain the risks and benefits of surgery versus no surgery. Those without symptoms should be told in detail about the early symptoms so that they can come back if and when they get symptomatic without any delays.
On the other hand patients with symptoms from gall stones should not wait as they are at risk of complications which can at times be life threatening. Here the specialist has to dissuade the patient from falling prey to ineffective 'guaranteed' remedies (usually offered by quacks).
Cancer and Gall Stones
Primary cancer of the gall bladder is rare. The risk at 0.5% with stones is low but the treatment for gall bladder cancer is unsatisfactory and survival is not good. It is usually seen in patients with a non-functioning gall bladder containing stones. Sometimes gallbladder tumours are an incidental finding during surgery for stones. They carry a poor prognosis, but this is partly because about half of gallbladder cancer is actually spread at the time of diagnosis. Stones more than 1 cm in size have a higher chance of being associated with cancer especially in patients older than 60 years who have had the problem for a long time.
Making a diagnosis
Because gall stones are so common they have been blamed for many digestive symptoms, but they are probably innocent in most cases. This concept is particularly important because ultrasonography is widely used in investigating patients and asymptomatic gall stones are often an incidental finding.
True symptoms of gall stones include
- acute cholecystitis (a febrile illness with pain in right upper part of tummy),
- biliary colic (pain in top centre of the tummy),
- jaundice (often painful), and
- acute pancreatitis.
Biliary colic is the commonest form of announcement by the stones that they are ready for treatment. It consists of clear cut, well remembered attacks of severe upper abdominal pain lasting at least half an hour. All these patients need specific investigation, and since gall stones usually occur in the gall bladder this is the logical place to begin. The advent of ultrasonography has simplified investigation. Definite gall stones are seen as sono-dense mobile areas within the gall bladder and throw an acoustic shadow. Sometimes stones are not mobile, in which case they are not easy to discriminate from unimportant polyps, and very small ones may be missed or fail to throw a helpful acoustic shadow. Ultrasonography can also allow measurement of the diameter of the common bile duct and show the liver ducts.
Treatment
When gallbladder stones are proved to be the cause of severe symptoms, cholecystectomy is the best treatment for most patients. The introduction of laparoscopic cholecystectomy over the past 10 years has changed surgical practice greatly. The procedure itself is associated with a more rapid return to work after what is usually a shorter hospital stay.
Surgical options
-
Traditional open surgery is done in many centres mainly by surgeons who do not have laparoscopic equipment or the training to do so. It is also indicated in cases of (a) bile duct stones, (b) complicated cases, (c) patients with heart and lung diseases who cannot tolerate anesthesia for laparoscopic surgery, and (d) patients with gall bladder cancer. After a straight forward uncomplicated operation, the patient usually goes home after 5 days.
-
Mini- Cholecystectomy is traditional surgery through a small cut, which is suitable in some patients who are thin and have an early disease. The view during this approach is very limited due to the small cut and hence there can be a very high incidence of complications if the surgeon is not careful. After a straight forward uncomplicated operation, the patient usually goes home after 3 days.
-
Laparoscopic Cholecystectomy is now the standard worldwide accepted mode of treatment for 'gall bladder stones that are causing trouble'. This is done through four small holes made on the tummy one of which is used to put a telescope in to look inside while other holes are used to put in instruments to free and remove the gall bladder with the stones inside them. After a straight forward uncomplicated operation, the patient usually goes home on the next day. If you would like to watch a very brief video clip of a laparoscopic operation, click here.
-
Micro/Mini Laparoscopic Cholecystectomy (click to know more about it) is a further advancement of the above technique using even smaller holes and narrower instruments and telescopes. Here there are no stitches on the skin in addition to the other advantages of standard laparoscopy. Pain too is less and recovery slightly faster. This technique led to slightly smaller cuts. Apart from its cosmetic appeal to some, there is no advantage in terms of pain and return to work.
-
NOTES ( Natural orifice transluminal endoscopic surgery ) is an experimental surgical technique whereby "scarless" abdominal operations can be performed with an endoscope passed through a natural orifice (mouth, urethra, anus, vagina etc.) then through an internal incision in the stomach, vagina, bladder or colon, thus avoiding any external incisions or scars. There are reports of it being successfully done in humans but the procedure has not gained popularity due to the risks of complications.
- SILS ( Single incision laparoscopic surgery ) , also known as Single port access (SPA) surgery, laparo endoscopic single-site surgery (LESS) or one port umbilical surgery (OPUS) or single port incisionless conventional equipment-utilizing surgery (SPICES) or natural orifice transumbilical surgery (NOTUS), or Embryonic Natural Orifice transumbilical surgery (E-NOTES) is an advanced minimally invasive surgical procedure in which the surgeon operates almost exclusively through a single entry point, typically the patient’s navel.
Since the entire surgery is performed through the navel, it does not leave any visible scar like a traditional multi-port laparoscopic approach. Surgeons employing this technique contend that patients should benefit from less post-operative pain, less blood loss, faster recovery time, fewer complications, and better cosmetic results. Below is a brief video of the procedure.
There is less pain, chances of infection is reduced to 25% as there is one cut compared to four earlier, less need of medications, and possibly early return to routine activities. It is a cosmetic delight to the younger age scar conscious population. One of my patient is a school girl who I think was the happiest of all the patients we have had.
We would like to call it "Cosmetic Laparoscopy" as suggested by one of our patients. The procedure can be readily learned and performed by laparoscopic surgeons without the need for expensive or experimental equipment. Using a single portal of entry to the abdominal cavity, the umbilicus, cosmesis, and scar reduction is achieved.
Cost of Surgery
The cost of surgery varies from place to place and hospital to hospital.
- In a government hospital it is supposed to be free but often the patient is asked to buy disposable instruments, consumables and some of the medicines. This could mean an expense varying from Rs 3000 if you are lucky to Rs 10000 if you are unlucky. Also there could be a common problem of equipment being out of order and long waiting lists.
- In a small nursing home with basic facilities and minimal overhead expenses, the cost could be around Rs 6000 for the treatment plus another Rs 4000 for medicines. Some times the nursing home offers package deals of about Rs 10,000 on a total door to door cost. Medically fit patients with uncomplicated early disease are ones who benefit most from these centres.
- In a larger nursing home (often called hospitals), that have more staff and facilities, the cost goes
up to the range of 15 to 20,000 rupees.
- Large private hospitals have a wide range of cost choice for the patients depending upon their choice of rooms ( general ward, shared rooms and private rooms ). Here the cost could range from Rs 35,000 to 55,000. Most patients who have associated medical problems or long standing disease prefer to go to these centres as they have more monitoring facilities, larger surgical and anesthesia teams, medical super specialists and intensive care facilities in case their need arises.
Non surgical treatment of gall bladder stones
If a patient with gallbladder stones refuses surgery or is unsuitable for a general anaesthetic, alternatives may need to be considered.
- Bile acid therapy is an attractively safe option but is suitable for only a few patients and is unsuitable in those with severe recurrent symptoms. The gall bladder must be functioning, and this can be best be shown by an oral cholecystogram. Really good results are achieved only with radiolucent stones of 5 mm or less in diameter. Stone dissolution needs to be verified by two normal ultrasound scans. Recurrence of stones after treatment can be expected within 5 years in about 40% of patients, who may then require further treatment. The best bile acid therapy currently available is probably ursodeoxycholic acid. Larger stones do not respond nearly as well, and bile acid therapy is not generally advised in patients with gallbladder stones that are more than 10 mm in diameter. Bile acid therapy also has a role in stone prevention in very high risk groups. It should be given during rapid weight reduction in morbidly obese people. There is unfortunately a 12% recurrence rate every year from this treatment.
- External shock wave lithotripsy has been used successfully in some highly
specialized centres, but this treatment often leaves fragments that have to be cleared by subsequent bile acid therapy. About one third of patients will experience colic as a direct result of external shock wave lithotripsy.
- Stone dissolution by gallbladder puncture and putting in of chemicals such as MTBE (methyl-tertiary-butyl-ether) is even more unusual. This does work, but is restricted to a very few skilled operators. It also has the risk of spill and destruction of the lining of gall bladder. It is a toxic chemical and is being used on experimental basis in a few centres in the world.
- A rotary mechanical lithotripter been tried in a few centre. It is like a 'mixie' which is introduced into the gall bladder by a puncture on the skin and the instrument grinds the stones which is then sucked out. This too has a risk of damaging the lining and causing perforation.
Results
Gallbladder surgery cures biliary colic, and it largely prevents attacks of acute pancreatitis. Obviously, the patient cannot get acute cholecystitis again. The results for other symptoms are less satisfactory. One year after cholecystectomy 50% of patients complain of digestive symptoms of some kind, so it is important to ensure that their expectations are realistic before surgery and also the surgery is being done for a symptom due to gall stones. The small number of patients whose symptoms do not improve at all or actually worsen after surgery are a more difficult problem. Some of these patients will be discovered to have retained, recurrent, or primary common bile duct stones and can be cured by their removal. A few patients may have biliary dyskinesia, which is improved by sphincterotomy. However, there are many other patients who remain discontented after surgery, who have no satisfactory explanation for their symptoms, and in whom treatment is generally ineffective.
As usual with medical progress, new problems emerge with changing practice. Now that gall stones can be diagnosed easily, the question is: "Do they really matter?" Most do not, and care is needed in evaluation for treatment of those that do matter to be able to get the best results.


