Photo curtesy of:
Alvarado Center for Surgical Weight Control
"Copyright: Alvarado Center for Surgical Weight Control, A Medical Group, used by permission."
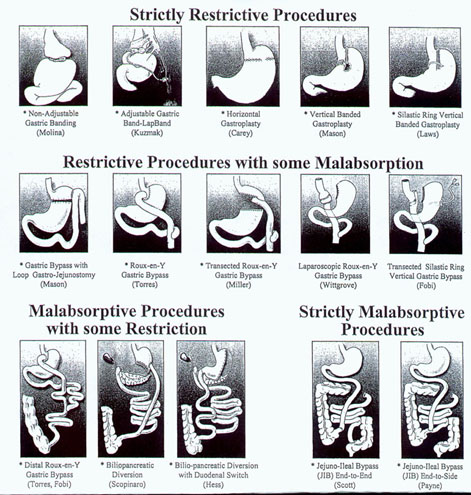
Open Roux en Y (Rny) (Restrictive with some Malabsorption)
Roux-en-y Gastric Bypass Surgery offers a successful combination of weight control with minimal nutritional or other risk, when follow up and nutritional guidelines are followed. Many obesity experts consider the surgery to be the "Gold Standard" of modern obesity surgery the benchmark to which other bariatric operations are compared. The operation achieves its effects by creating a very small stomach, from which the rest of the stomach is divided and separated. ISome surgeons do not divide just staple) The small intestine is "attached" to the new stomach, allowing the lower pan of the stomach to be bypassed. A thorough description, including diagrams, of the operation will be provided to you during your consultation or as part of the free seminar we encourage potential patients to attend. Suffice to say, that no bodily functions are altered as a result of the operation, and it is completely reversible if it ever needed to be. Complete descriptions with illustrations of the surgery are presented by your surgeon at time of consultation. Following surgery, there is little interference with normal absorption of food. The operation restricts food intake and reduces the feeling of hunger. The result is an early sense of "fullness" followed by a sense of satisfaction. Even though the portion size is small (2 to 6 ounces per serving), there is no hunger and no sense of being deprived. Patients continue to enjoy eating all types of food after surgery. They just eat a much smaller portion than they used to. The Roux-en-y Gastric Bypass is an excellent tool for achieving longterm control of morbid obesity (the state of being 100 or more pounds over ideal body weight). Weight loss of 80-100% is achievable by most patients, as internal and external outcome studies demonstrate. And maintenance of that weight loss is likely with adherence to a straight forward behavior regimen.
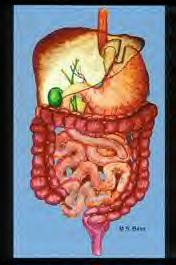
The Stomach is separated into two parts. The small Stomach pouch receives food. The lower part of the stomach received most of the gastric juices coming from the liver and other organs. The small intestine is carefully measured and cut. One end is connected to the small stomach pouch. The other end is reconnected to the small intestine, forming a "Y".
The Roux-en-Y Gastric Bypass Surgery helps you lose weight in three ways...
1. You eat less (Volume restriction) With a separate small stomach pouch, you feel full after eating a small amount of food. This approach is much more effective in restricting food volume than other surgical techniques, such as stomach stapling.
2. Your appetite changes (Behavior modification) The procedure reinforces a change in your eating habits. After the procedure, most patients find that their body will not easily tolerate foods that are high in refined sugars and fats. With this built-in control, called "the dumping syndrome," which produces short-term discomfort and flu-like symptoms, you naturally learn to avoid these foods. (Our Bariatric Treatment Centers nutritionists help you avoid the foods that may cause discomfort and help you choose from a wide variety of foods you can enjoy.) Other surgical procedures don't provide this important benefit of behavior modification.
3. You absorb fewer calories (Malabsorption) Food bypasses part of the small intestine and digestion occurs in the lower part of the small intestine. These two factors reduce the amount of calories your body absorbs from the food you eat.
The reduced stomach pouch size, change in eating habits and absorption of fewer calories allow patients to be successful at long-term weight loss, as opposed to short-term weight loss programs or diets that rely on willpower, costly meal replacements, or dietary supplements.
Please discuss ahead of time with your selected surgeon if the RNY will be a transectioned (divided/seperated) procedure ..You don't want the staples to migrate and regain your weight down the road this is an important question for your surgeon.
====================================================
Laparoscopic Roux-en-Y
same as open Roux-en-Y except instead of opening you with a long incision on your stomach, Surgeons use a pencil thin optical telescope, to project a picture to a TV monitor. Having surgery this way, smaller scars , usually 3 to 4 small incisions. Quicker recovery time and less pain.
====================================================
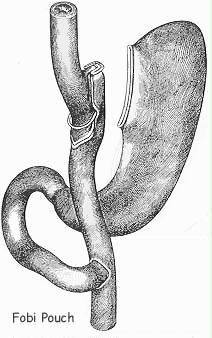
Fobi Pouch (Restrictive with Malabsorption)
The Fobi procedure (Divided RNY) creates an approximately 1 oz. vertically-oriented, banded pouch, completely cut away from the remaining stomach and connected to the small intestine in a Roux-n-y fashion with a jejunal interposition.
A vertically-oriented pouch is much less prone to stretching than the conventional horizontally-oriented pouch. The band at the outlet of the pouch enforces a small fixed outlet, slowing the time it takes for food to pass through the pouch and, therefore, the amount of food that can be comfortably eaten in a day. Cutting the pouch completely away from the rest of the stomach and interposing small intestine (jejunum) between the cut edges minimizes the chance of the stomach growing back together and reversing the bypass. Fobi Pouch can be done Proximal, medial and distal depending on the beginning weight patient..Discuss this with your surgeon.
The Fobi Pouch Gastric Bypass is characterized by:
• A Small 1 oz Stomach Pouch 1 to 1.5 oz when mature.
• A Small Controlled, Non-Stretchable Outlet
• An Acceptably Low Complication Rate
• Satisfactory Weight Loss 70% most 100%
• Absence of Excessive Late Failures . Total regain of weight — which can occur in a substantial percentage of patients undergoing vertical banded gastroplasty or classic gastric bypass — is very uncommon with the Fobi pouch procedure
=======================================================
Distal Gastric Bypass (Restrictive with greater Malabsorption)
The Gastric Bypass operation can be modified, to alter absorption of food, be moving the Y-connection downstream ("distally"), effectively shortening the bowel available for absorption of food. The weight loss effect is then a combination of the very small stomach, which limits intake of food, with malabsorption of the nutrients which are eaten, reducing caloric intake even further. Patients have increased frequency of bowel movements and increased fat in their stools (bowel movements). The odor of bowel gas is very strong, which can cause social problems or embarrassment. Calcium absorption may be impaired, as well as absorption of vitamins, particularly those which are soluble in fat (Vitamins A, D, and E). Vitamin supplements must be used daily, and failure to follow the prescribed diet and supplement regimen can lead to serious nutritional problems in a small percentage of patients. We. and others, have noted an increased incidence of ulcers post-operatively, in patients having this procedure.
This operation is often confused with the Roux-en-Y Gastric Bypass. It is however, much closer to the biliopancreatic diversion. This operation attempts to combine a gastric restrictive and malabsorbtive procedure. A small gastric pouch is formed and over 50% of the small intestine is bypassed. This lends itself to a higher degree of protein-calorie malabsorbtion and marginal ulcer formation than the biliopancreatic diversion. Fortunately, in this case, the stomach pouch will continue to increase in size as long as the patient is encouraged to overeat.
====================================================
Biliopancreatic Diversion (BPG)
This very powerful operation involves removal of approximately 2/3 of the stomach, and re-arrangement of the intestinal tract so that the digestive enzymes are diverted away from the food stream, until very late in its passage through the intestine. The effect is to selectively reduce absorption of fats and starches, while allowing near-normal absorption of protein, and of sugars. Calorie intake is much reduced, even while normal-sized food portions are eaten.
This operation was described in Italy in 1973 and is still being performed in a few centers. This operation consists of removing part of the stomach, leaving a 200-250 cc pouch and shortening the small intestinal food conduit to 250 cm. There is a 50 cm common channel in which bile and pancreatic digestive juices mix prior to entering the colon. Weight loss occurs as a result of "dumping" most of the calories and nutrients into the colon where they are not absorbed. There is need for precise control of types of food ingested and an emphasis on protein load. Most patients require life-long nutritional supplements which can be quite expensive. Blood tests are required every few months. Weight loss has not been shown to be superior to the restrictive operations. The social aspects of intestinal gas, diarrhea and odor can be devastating. Most insurance companies will not authorize this type of procedure because of the high complication rates and metabolic problems following this procedure. Although this operation is very powerful, patients are subject to increased risk of nutritional deficiencies of protein, vitamins and minerals. Vitamin supplementation recommendations must be carefully followed, and dietary intake of protein must be maintained, while intake of fat must be limited. Patients are annoyed by frequent large bowel movements, which have a strong odor. Excess fat intake leads to irritable bowel symptoms, and may lead to rectal problems.
Common to all malabsorbtive procedures is the apparent shortening of the intestine in contact with food. Although seemingly logical at first, making the system less efficient in its absorption of nutrients requires continued overindulgence by the patient for survival. The "eat to live" configuration can be quite harmful if adequate volumes of food were not available or if you were to contract a simple case of the "flu". Because of the shortened intestinal tract, hospitalization may be required and therefore travel to certain countries that do not have the medical facilities here in the United States should be discouraged. Iron, calcium, protein, vitamin and mineral deficiencies mandate continued supplements and occasional intravenous therapy. The Site listed below states: That they do not perform the malabsorbtive procedures as they have not found convincing evidence that they provide a more consistent weight loss or improved quality of life. They have converted many of these procedures to the Roux-en-Y Gastric Bypass because of severe metabolic complications and malnutrition.
There are many other procedures that are touted as "unique". They are only presenting common procedures with known tract records and definable statistics. They advise you to use common sense in your educational process. If it sounds too good to be true, it generally is.
Jejuno-ileal Bypass
This operation is of historic importance. This prototypical malabsorbtive procedure was performed from 1963 to 1980. The amount of small intestine in contact with food was severely shortened. Although this procedure was quite simple to perform, the metabolic complications were devastating. Protein-calorie malabsorbtion, diarrhea, vitamin and mineral deficiencies were common. In addition, kidney failure has been seen in patients ten years out from surgery. It is because of this failed procedure, that many physicians and insurance companies look down on all bariatric procedures.
BPD/DS
BilioPancreatic Diversion with Duodenal Switch
The procedure is a combination restrictive-malabsorptive procedure as well, except that the main mechanism of weight loss and maintenance is malabsoprtion, with restriction playing a much lesser role. Only the downstream 40% of small intestines is used to absorb food in this procedure, and only about one third of this is able to absorb fats and starches. The remainder of the small intestine carries the digestive juices from the liver and pancreas (the biliopancreatic flow), and as previously noted, only to the last 100cm (approx 3 feet) of food-carrying intestine. It is the 60% shortening of the intestine that initiates the weight loss and the diversion of the biliopancreatic flow which maintains that loss long-term. The stomach volume is reduced by approximately 75%, to act as a temporary restrictive effect short-term, and, more importantly, to prevent ulcers from forming long term. With the duodenal switch mechanism, the natural emptying mechanism of the stomach is preserved, eliminating the "dumping syndrome" and resulting in essentially normal eating abilities 6 months after surgery in most patients. The re-arrangement of the small intestine allows patients to eat normal volumes of food because an absorption threshold for fat and starches is established due to the biliopancreatic diversion which cannot be overeaten. The excess non-digested food is passed in the stool.
Patients undergoing biliopancreatic diversion/duodenal switch eat normally and have bowel habit changes characterized by frequent (2-4 per day) soft stools and a propensity for gas. Both of which are generally malodorous unless a stool deodorant (such as Devrom) is taken.
A: The stomach is trimmed to a 4-6 ounce volume, preserving its natural inlet and outlet ( the pylorus). This results in a temporary restrictive effect on eating for several months, which then reverts to normal, as well as decreasing the incidence of ulcer formation after surgery.
B: The small intestine that the stomach normally empties into the duodenum is "switched" to the downstream portion of the small intestine (the digestive limb-D). The outflow from the duodenum, carrying the digestive juices and enzymes (but no food) becomes the bilio-pancreatic limb
C: utilizing approximately 60% of the small intestines length.
D: The digestive limb takes up approximately 40% of the small bowel length, and most of this length is upstream from where the biliopancreatic limb deposits its juices to allow for the absorption of fats and starches.
E: The common limb, being the portion of intestine where both food and biliopancreatic outflow meet, is made up of the most downstream 100 cm of small intestine and is the only portion where absorption of dietary starches and fats occurs, which is not very much. The capacity for absorption reaches a maximum within several months after surgery and cannot be over eaten.
F: The gallbladder and appendix are removed.
Note that a rather large stomach remnant is provided for eating, loosing its restrictive effect over time, but that this normal food volume is digested over only 40% of the intestine length. This arrangement is increasing primarily malabsorptive and only partially restrictive
Dr. Husted reserves this procedure for the SUPER OBESE those over 400 pounds... Although will make acception if patient driven.. This procedure has proven to me successful in the super obese.. Strict adherence to the vitamin and supplements regiment is crucial in this procedure as in any malabsorption procedure...
Please visit Dr. Husted's webpage below for more information on this procedure..
John D. Husted, M.D...Cumberland Center for Obesity Surgery
==================================================
Adjustable Gastric Band (AGB) (Restrictive)
Gastric Banding is a variation on the gastroplasty, in which the stomach is neither opened nor stapled -- a band is placed around the outside of the upper stomach, to create an hourglass-shaped stomach, and to produce a small pouch with a narrow outlet. The special device used to accomplish this is made of implantable silicone rubber, and contains an adjustable balloon, which allows us to adjust the function of the band, without re-operation. This device enjoys considerable advantage over the standard gastroplasty:
It can be inserted laparoscopically, without the usual large incision. It does not require any opening in the gastrointestinal tract, so infection risk is reduced. There is no staple line to come apart. It is adjustable.
====================================================
Loop Gastric Bypass
This form of Gastric Bypass was developed years ago, and has generally been abandoned by most bariatric surgeons as unsafe. Although easier to perform than the Roux en-Y, it creates a severe hazard in the event of any leakage after surgery, and seriously increases the risk of ulcer formation, and irritation of the stomach pouch by bile. Most bariatric surgeons agree that this operation is obsolete, and should remain defunct. This operation has been resurrected, in order to make the laparoscopic procedure easier to perform. A fundamental principle of laparoscopic surgery is that the operation should not be compromised or degraded, in order to accomplish it using limited access techniques. The loop bypass does not meet this standard....
===================================================
Gastroplasty
Gastroplasty, or Stomach Stapling (Gastric Partitioning) is widely performed in the United States and elsewhere. It is a technically simple operation, accomplished by stapling the upper stomach, to create a small pouch, about the size of your thumb, into which food flows after it is swallowed. The outlet of this pouch is restricted by a band of synthetic mesh, which slows its emptying, so that the person having it feels full after only a few bites (one thumbful) of food. Characteristically, this feeling of fullness is not associated with a feeling of satisfaction- the feeling one has had enough to eat.
Patients who have this procedure,because they seldom experience any satisfaction from eating, tend to seek ways to get around the operation. Trying to eat more causes vomiting, which can tear out the staple line and destroy the operation. Some people discover that eating junk food, or eating all day long by "grazing" helps them to feel more sense of satisfaction and fulfillment -- but weight loss is defeated. In a sense, the operation tends to encourage behavior which defeats its objective.
Overall, about 40% of persons who have this operation never achieve loss of more than half of their excess body weight. In the long run, five or more years after surgery, only about 30% of patients have maintained a successful weight loss. Many patients must undergo another, revision operation, to obtain the results they seek.
****************************************************
Restrictive Procedures
These procedures do not bypass any intestine there is no malabsortion of any kind..
ABG-- Adjustable Banded Gastroplasty. Developed at Huddinge University Hospital in the 1980’s. It was designed to restrict food intake. No malabsorption is involved. This is procedure is reversable because no cutting of organs is involved. You simply remove the band. Aftercare is a must to insure proper adjustment of the band. The Laparoscopic Banding has not been approved by the FDA in the United States yet.
VBG--Vertical Banded Gastroplasty. This is a restrictive procedure, first introduced in the U.S. in 1982. A small pouch is created to restrict food intake. No changes are made to the intestines. 40-60% of excess weight loss is generally achieved. This procedure cannot be reversed though it can be revised. It does have a history of high percentage of repeat surgeries due to failure and complications.
Information from this webpage used by permission from
Alvarado Center for Surgical Weight Control
Academy of Bariatric Surgeons
VICTORIA'S RECIPES FOR GASTRIC BYPASS PATIENTS
Click on the above book to visit my cookbook page
****************************************************
Looking for a surgeon in your area? Click on the below link for a clickable by state map!!
Bariatric Surgery Resources By States
Visit my main "GASTRIC BYPASS WEBSITE"
Gastric Bypass Information, Links & Recipes
Also visit my Gastric Bypass Cookbook webpage below
VICTORIA'S RECIPES FOR GASTRIC BYPASS PATIENTS

Powered by counter.bloke.com
![]()
Free search engine submission and placement services!