Multifascicular
Blocks
The term multifascicular block refers to conduction delay in more than one of the structural components of the specialized conduction system, that is, the left bundle branch, the left anterior and posterior fascicles, and the right bundle branch. Conduction delay in any two fascicles is called bifascicular block, and delay in all three fascicles is called trifascicular block.
Bifascicular block can have several forms, including RBBB with LAFB, which is characterized by the ECG pattern of RBBB plus left axis deviation beyond – 45 degrees, or RBBB with LPFB, with an ECG pattern of RBBB and a mean QRS axis deviation to the right of + 120 degrees. LBBB is often considered to reflect unifascicular block, although as discussed above, it can result from delay in both the anterior and posterior fascicles. This paradox represents one of the inadequacies of current ECG terminology and the simplification inherent in the trifascicular schema of the conduction system.
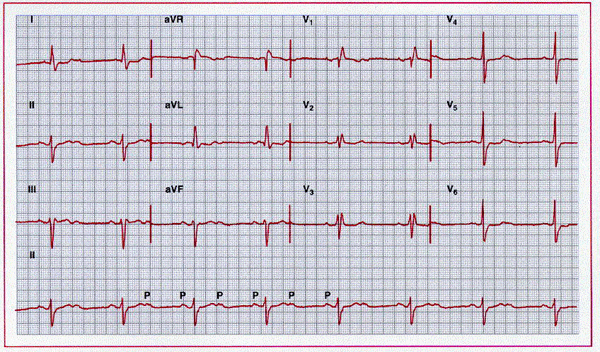
Sinus rhythm at 95 beats/min with 2:1 atrioventricular
block. Conducted ventricular beats show a pattern consistent with bifascicular
block with delay or block in the right bundle and left anterior fascicle. The
patient underwent pacemaker implantation.

Sinus rhythm with a 2:1 atrioventricular block. QRS
morphology in the conducted leads is consistent with bifascicular block with
delay or block in the right bundle and left posterior fascicle. Subsequently,
complete heart block was also noted. The patient underwent pacemaker
implantation.
Trifascicular block involves conduction delay in the right bundle branch plus delay in either the main left bundle branch or both the left anterior and the left posterior fascicles. The resulting ECG pattern is dependent on (1) the relative degree of delay in the affected structures and (2) the shortest conduction time from the atria to the ventricles through any one fascicle. Ventricular activation begins at the site of insertion of the branch with the fastest conduction time and spreads from there to the remainder of the ventricles. For example, if delay in the right bundle branch is less than the delay in the left main bundle branch, activation will begin in the right ventricle and the QRS pattern will resemble that of LBBB. If the delay were greater in the right bundle branch than in the left bundle branch, the ECG pattern would be that of RBBB. The fascicle with the greatest delay can vary with, for example.
|

What distinguishes ECG patterns of trifascicular block from those of bifascicular block is an increased overall AV conduction interval that results specifically from prolongation of the His-ventricular time. In bifascicular block, conduction time through the unaffected fascicle (and hence, overall AV conduction time) is normal. In trifascicular block, however, the delay in conduction through even the least affected fascicle is abnormal and results in relative prolongation of the overall AV conduction interval. (Note that only delay, not block of conduction is required. If block were present in all fascicles, conduction would fail and complete heart block would result. This situation is perhaps best illustrated by cases of alternating bundle branch block; if the block were total in one bundle branch, development of block in the other would produce complete AV block rather than a change in bundle branch block patterns.) Thus, a diagnosis of trifascicular block requires an ECG pattern of bifascicular block plus evidence of prolonged AV conduction.
Detecting AV conduction delay is best accomplished by intracardiac recordings as a prolongation of the H-V interval. On the surface ECG, AV conduction delay may be manifested as a prolonged PR interval. However, the PR interval includes conduction time in the AV node, as well as in the intraventricular conduction system. Prolonged intraventricular conduction may be insufficient to extend the PR interval beyond normal limits, while a prolonged PR interval can reflect concomitant delay in the AV node rather than in all three intraventricular fascicles. Thus, the finding of a prolonged PR interval in the presence of an ECG pattern of bifascicular block is not diagnostic of trifascicular block, while the presence of a normal PR interval does not exclude this finding.
The major clinical implication of a multifascicular block is its relation to advanced conduction system disease. It may be a marker for advanced myocardial disease and may identify patients at risk for heart block.