Intraventricular
Conduction Delays and Preexcitation
Under normal conditions, activation of the left ventricle begins simultaneously at the insertion sites of the fascicles. Delayed conduction in a fascicle—fascicular block—results in activation of these sites sequentially rather than simultaneously and produces an abnormal sequence of early left ventricular activation. This altered sequence produces characteristic ECG patterns. Even modest delays in conduction through the affected structure may be enough to alter ventricular activation patterns sufficiently to produce characteristic ECG patterns; complete block of conduction is not required.
LEFT ANTERIOR FASCICULAR BLOCK
Damage to the left anterior fascicle is a very common occurrence because of the delicate nature of the structure. The most characteristic finding is marked left axis deviation. However, LAFB is not synonymous with left axis deviation. Axis shifts to between – 30 and – 45 degrees commonly reflect other conditions, e.g., LVH, without conduction system damage and are best referred to as left axis deviation rather than LAFB.
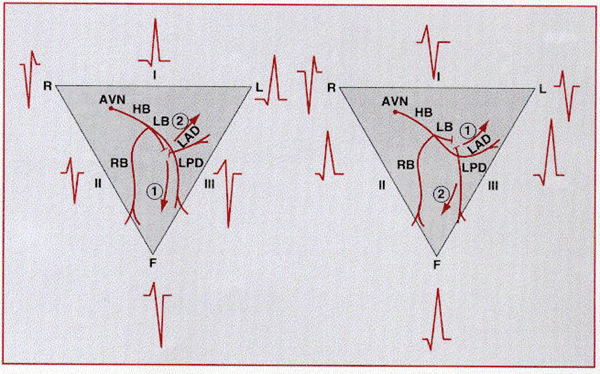
Diagrammatic representation of fascicular blocks in left
ventricles. Interruption of the left anterior fascicle (LAF) (left) results in
an initial inferior (1) followed by a dominant superior (2) direction of
activation; interruption of the left posterior fascicle (LPF) (right) results in
an initial superior (1) followed by a dominant inferior (2) direction of
activation. AVN = atrioventricular node; HB = His bundle; LB = left bundle; RB =
right bundle.
Left axis shift is a result of delayed activation of the anterosuperior left ventricular wall. Delayed activation causes unbalanced inferior and posterior forces early during ventricular activation and unopposed anterosuperior forces later during the QRS complex. The abnormal pattern results in initial r waves followed by deep S waves in the inferior leads (left axis deviation with rS patterns) and a qR pattern in left-looking leads (leads aVl and usually V5 and V6). Initial q waves in these leads reflect the normal left-to-right activation of the septum. The overall QRS duration is not prolonged; fascicular block only alters the sequence of left ventricular activation but does not by itself prolong the overall duration of ventricular excitation or the QRS complex. LAFB usually does not produce prominent changes in the precordial leads. V1 and V3 are usually unchanged; V4 through V6 commonly show deep S waves related to superiorly directed late QRS forces.
LAFB is common in persons without overt cardiac disease, as well as a wide range of diseases, and has minimal or no independent prognostic significance. Commonly associated cardiac and systemic conditions include myocardial infarction, especially occlusion of the left anterior descending coronary artery,LVH, hypertrophic and dilated cardiomyopathy, and degenerative diseases. The development of LAFB with rS complexes in II, III, and aVf can mask the Q waves of a prior inferior myocardial infarction.
LEFT POSTERIOR FASCICULAR BLOCK.
Conduction delay in the left posterior fascicle is considerably less common than delay in the anterior fascicle because of its thicker structure and more protected location near the left ventricular inflow tract. The conduction delay results in sequential activation of the anterosuperior left ventricular free wall, followed by activation of the inferoposterior aspect of the left ventricle, that is, the reverse of the pattern observed with LAFB.
reflect this altered activation pattern. Right axis deviation with rS patterns in leads I and aVl, as well as qR complexes in the inferior leads, is the result of early unopposed activation forces from the anterosuperior aspect of the left ventricle (producing the initial q and r waves) and late unopposed forces from the inferoposterior free wall (generating the late S and R waves). As in the case of LAFB, the overall activation time of the ventricles is not prolonged and the QRS duration remains normal.
LPFB, like LAFB, can occur in almost any cardiac disease but is unusual in otherwise healthy persons. Other conditions that enhance electrical forces from the right ventricle, such as right ventricular enlargement and extensive lateral infarction, can produce similar ECG patterns and must be excluded before a diagnosis of LPFB is made.
Left bundle branch block (LBBB) results from conduction delay or block in any of several sites in the intraventricular conduction system, including the main left bundle branch, in each of the two fascicles, or less commonly, within the fibers of the bundle of His that become the main left bundle branch. The result is extensive reorganization of the activation pattern of the left ventricle.
LBBB produces a prolonged QRS duration, abnormal QRS complexes, and ST-T wave abnormalities.Basic requirements include a prolonged QRS duration to 120 milliseconds or beyond; broad, sometimes notched R waves in leads I and aVl and the left precordial leads; narrow r waves followed by deep S waves in the right precordial leads; and absent septal q waves. R waves are typically tall and S waves are deep. The mean QRS axis with LBBB is highly variable; it can be normal or deviated to the left. Left axis deviation is associated with more severe conduction system disease that includes the fascicles as well as the main left bundle.In addition to these features, some electrocardiographers require a delayed intrinsicoid deflection (³60 milliseconds) to diagnose LBBB.
|
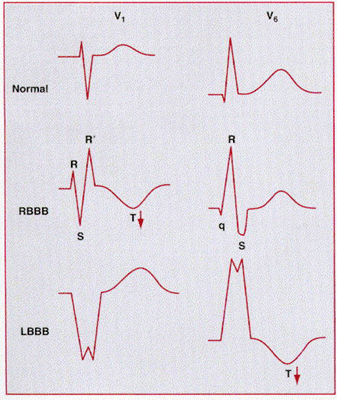
ST-T wave changes are also prominent with LBBB. In most cases, the ST wave and the T wave are discordant with the QRS complex; that is, the ST segment is depressed and the T wave is inverted in leads with positive QRS waves (leads I, aVl, V5, and V6), while the ST segment is elevated and the T wave is upright in leads with negative QRS complexes (leads V1 and V2).
An incomplete form of LBBB may result from lesser degrees of conduction delay in the left bundle branch system. Left ventricular activation begins, as in complete LBBB, on the right side of the septum, but much of left ventricular activation occurs through the normal specialized conduction system. ECG features include (1) loss of septal q waves (reflecting reversal of the normal pattern of septal activation), (2) slurring and notching of the upstroke of R waves (because of the presence of competing activation fronts), and (3) modest prolongation of the QRS complex (between 100 and 120 milliseconds).
MECHANISMS
FOR ECG ABNORMALITIES
The ECG abnormalities of LBBB result from an almost completely reorganized pattern of left ventricular activation. Initial septal activation occurs on the right (rather than on the left) septal surface, and right ventricular excitation occurs earlier than normal. This sequence of septal activation results in the absence of normal septal q waves in the ECG.
The excitation wave then spreads slowly, by conduction from muscle cell to muscle cell, to the left side of the septum; the earliest left ventricular activation begins as late as 30 to 50 milliseconds into the QRS complex. Endocardial activation of the left ventricle may then require an additional 40 to over 180 milliseconds, depending largely on the functional status of the distal left bundle and Purkinje systems.Thus, the overall QRS complex is prolonged and can be very wide in patients with, for example, ventricular scarring from prior myocardial infarction. Once left ventricular activation begins, it proceeds in a relatively simple and direct manner around the free wall and, finally, to the base of the heart. Direct progression of activation across the left ventricle projects continuous positive forces to left-sided leads and continuous negative ones to right-sided leads. Spread predominantly through working muscle fibers rather than the specialized conduction system results in notching and slurring as a consequence of discontinuous anisotropy, as described above.
The discordant ST-T wave pattern is a result of the transventricular recovery gradients referred to above. With LBBB, the right ventricle is activated and recovers earlier than the left, so recovery vectors or dipoles are directed toward the right and away from the left. Hence, positive ST-T waves will be registered over the right ventricle and negatives ones over the left ventricle. These transventricular gradients play only a minor role in normal conduction because the simultaneous activation of multiple regions cancels the forces that they produce; with bundle branch block, activation is sequential, so cancellation is reduced. Because the ST-T wave changes with LBBB are generated by abnormalities in conduction, they are called secondary T wave abnormalities; as will be discussed below, ST-T wave changes produced by direct abnormalities of the recovery process are referred to as primary T wave abnormalities.
LBBB usually appears in patients with underlying heart disease. It is associated with significantly reduced long-term survival, with 10-year survival rates as low as 50 percent, probably reflecting the severity of the underlying cardiac disease. Among patients with coronary artery disease, the presence of LBBB correlates with more extensive disease, more severe left ventricular dysfunction, and reduced survival rates.Patients with associated left axis deviation have more severe clinical manifestations.The paradoxical combination of complete LBBB with right axis deviation has been reported as a marker of severe myocardial disease, especially dilated cardiomyopathy.
In addition to the hemodynamic abnormalities produced by these underlying conditions, the abnormal ventricular activation pattern of LBBB itself induces hemodynamic perturbations,including abnormal systolic function with dysfunctional contraction patterns, reduced ejection fraction and lower stroke volumes, and abnormal diastolic function; reversed splitting of the second heart sound and functional mitral regurgitation are common. In addition, functional abnormalities in phasic coronary blood flow and reduced coronary flow reserve caused by delayed diastolic relaxation often result in septal or anteroseptal defects on exercise perfusion scintigraphy in the absence of coronary artery disease.Pharmacological stress testing with dobutamine or adenosine may be more specific than exercise scintigraphy in diagnosing left anterior descending coronary stenosis in the presence of LBBB.
A major impact of LBBB lies in obscuring or simulating other ECG patterns. The diagnosis of LVH is complicated by the increased QRS amplitude and axis shifts intrinsic to LBBB; in addition, the very high prevalence of anatomical LVH in combination with LBBB makes defining criteria with high specificity difficult. The diagnosis of infarction may be obscured; as will be described, the emergence of abnormal Q waves with infarction is dependent on a normal initial sequence of ventricular activation, which is absent with LBBB. In addition, ECG patterns of LBBB, including low R wave amplitude in the midprecordial leads and ST-T wave changes, can simulate anterior infarct patterns.
RBBB is a result of conduction delay in any portion of the right-sided intraventricular conduction system. The delay can occur in the main right bundle branch itself, in the bundle of His, or in the distal right ventricular conduction system. The latter is the common cause of RBBB after right ventriculotomy performed, for example, to correct the tetralogy of Fallot. The relative fragility of the right bundle branch, as suggested by the development of RBBB after minor trauma produced by right ventricular catheterization, corresponds to the high prevalence of RBBB in the general population.
As with LBBB, the QRS complex duration exceeds 120 milliseconds. The right precordial leads show prominent and notched R waves with rsr, rsR´, or rSR´ patterns, while leads I, aVl, and the left precordial leads demonstrate wide S waves that are longer in duration than the preceding R wave. Septal q waves are preserved because the initial ventricular activation remains unchanged. The ST-T waves are, as in LBBB, discordant with the QRS complex, so T waves should be inverted in the right precordial leads (and other leads with a terminal R´ wave) and upright in the left precordial leads and in leads I and aVl.
The mean QRS axis is not altered by RBBB. Axis shifts can occur, however, as a result of the simultaneous occurrence of fascicular block along with RBBB. This concurrence of RBBB with either LAFB (producing left axis deviation) or LPFB (producing right axis deviation) is termed bifascicular block, as described below. Features indicative of incomplete right bundle branch block (IRBBB), produced by lesser delays in conduction in the right bundle branch system, are commonly seen. This finding is most frequently characterized by an rSr´ pattern in lead V1 with a QRS duration between 100 and 120 milliseconds.
MECHANISMS
FOR ECG ABNORMALITIES
With delay or block in the proximal right bundle branch system, activation of the right side of the septum is initiated after slow transeptal spread of activation from the left septal surface. The right ventricular free wall is then excited slowly, with variable participation of the specialized conduction system. The result is slowed and delayed activation of the right ventricle with much or all of the right ventricle undergoing activation after activation of the left ventricle has been completed. Consequently, the electrical forces generated by the right ventricle are not, as in normal conduction, canceled by the more powerful forces from the left ventricle and emerge in the ECG late in the QRS complex. In addition, because left ventricular activation remains relatively intact, the early portions of the QRS complex are normal. Delayed activation of the right ventricle causes prolongation of the QRS duration, while the late and unopposed emergence of right ventricular forces produces increased anterior and rightward voltage in the ECG. Discordant ST-T wave patterns are generated by same mechanisms as for LBBB; with RBBB, recovery forces are directed toward the earlier-activated left ventricle and away from the right. While these ECG changes of IRBBB are commonly attributed to conduction defects, they can reflect RVH without intrinsic dysfunction of the conduction system.
RBBB is a common finding in the general population, and many persons with it have no clinical evidence of structural heart disease. In this group without overt heart disease, the ECG finding has no prognostic significance. However, the new onset of RBBB does predict a higher rate of coronary artery disease, congestive heart failure, and cardiovascular mortality. When cardiac disease is present, the coexistence of RBBB suggests advanced disease with, for example, more extensive multivessel disease and reduced long-term survival in patients with ischemic heart disease.An apparently specific entity known as the Brugada syndrome has been described in which RBBB with persistent ST segment elevation in the right precordial leads is associated with susceptibility to ventricular tachyarrhythmias and sudden cardiac death.
RBBB interferes with other ECG diagnoses, although to a lesser extent than LBBB does. The diagnosis of RVH is more difficult to make with RBBB because of the accentuated potentials in lead V1. RVH is suggested, although with limited accuracy, by the presence of an R wave in lead V1 that exceeds 1.5 mV and a rightward shift of the mean QRS axis. The usual criteria for LVH can be applied but have lower sensitivities than with normal conduction. The combination of left atrial abnormality or left axis deviation with RBBB also suggests underlying LVH.