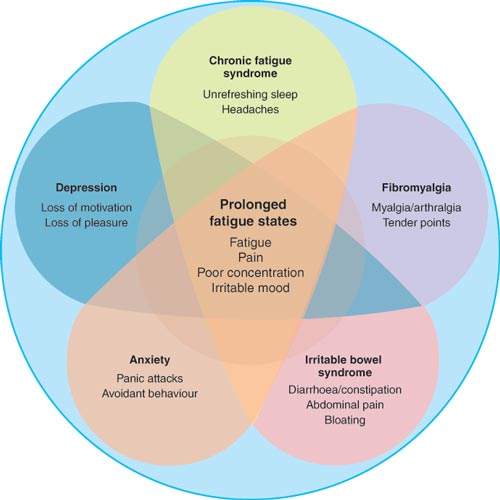
Syndromal diagnoses like CFS have a long history of use in clinical medicine. CFS by its nature cannot be classified medically as a disease and yet it is characterised by a set of "recognisable symptoms that cannot be attributed to any alternative condition"4. Symptoms of CFS are currently believed to be the result of disturbed brain function and the pathophysiology of CFS is currently unknown. Therefore, CFS is probably best regarded as "dis-ease"— a subjective state that can only be defined by reference to the person — rather than a "disease". As yet, no medication has been shown to provide long term remission or "cure" in people with CFS. Therefore, conventional medical treatments for CFS are empirical and careful monitoring is required to ensure that the symptomatic benefits outweigh any side effects. Furthermore, many people with CFS report an increased susceptibility to drug side effects4.
CFS is more common in women than men and in young adults. About 10-25% of patients presenting to general practitioners are diagnosed with CFS.
An Australian study in 2002 reports that excessive 50Hz magnetic field exposure may contribute to the symptoms of CFS and decreased immune function13.. (See the EMF article for more information on this)
Sick Building Syndrome (SBS) is also another environmental factor which needs serious consideration in CFS. According to the Health Protection Agency in Washington, the following can be causes:-
References:
1. 17th Edition of The Merck Manual of Diagnosis and Therapy
2. Murray, M & Pizzorno, J., The Encyclopedia of Nutritional Medicine, 2000, Little, Brown & Co. London, UK.
3. Fukuda K, Straus SE, Hickie I, et al. The chronic fatigue syndrome: a comprehensive approach to its definition and study. International Chronic Fatigue Sydnrome Study Group. Ann Intern Med 1994; 121: 953-959.
4. Chronic fatigue syndrome, Clinical practice guidelines — 2002, MJA 6 May 2002 176 (9 Suppl): S17-S55
5. Goldstein, J.A., Betrayal by the Brain, 1996, Haworth Medical Press, Binghampton, New York.
6. Childre, D.& Martin, H., The HeartMath Solution., 1999, Harpers Publishers, San Francisco.
7. Demitrack, M. A., et al. Evidence for impaired activation of the hypothalamic-pituitary-adrenal axis in patients with chronic fatigue syndrome. J Clin Endocrinol Metab. 73:1224-1234, 1991.
8. Lorensen, T. D. & Gow, K, M., Quantitative Electroencehalographic Comudulation: An investigation of patterns in Chronic Fatigue Syndrome., Journal of Neurotherapy, Vol. 7, No. 1, 3-18, 2003.
9. Loblay RH, Swain AR. The role of food intolerance in chronic fatigue syndrome. In: Hyde BM, editor. The clinical and scientific basis of myalgic encephalomyelitis/chronic fatigue syndrome. New York: The Nightingale Research Foundation, 1992.
10. Manu P, Matthews DA, Lane TJ. Food intolerance in patients with chronic fatigue. Int J Eat Disord 1993; 13: 203-209.
11. Aaron LA, Buchwald D. A review of the evidence for overlap among unexplained clinical conditions. Ann Intern Med 2001; 134: 868-881.
12. Jason LA, Taylor RR, Kennedy CL. Chronic fatigue syndrome, fibromyalgia, and multiple chemical sensitivities in a community-based sample of persons with chronic fatigue syndrome-like symptoms. Psychosom Med 2000; 62: 655-663.
13. Maisch, D., Podd, J. & Rapley, B., Changes in health status in a group of CFS and CF patients following removal of excessive 50Hz magnetic field exposure., J. Aust. Coll. Nutr. & Env. Med. Vol. 21. No. 1. April 2002
14. In-Tele-Health., Hyperhealth - Natural Health and Nutrition CD ROM- Fitzroy, Victoria. 2004.
15. Bou-Holaigah, I., et al., The relationship between neurally mediated hypotension and the chronic fatigue syndrome. JAMA, 274(12):961-7, 1995.
16. Jacobson, W., et al., Serum folate and chronic fatigue syndrome., Neurology, 43(12):2645-7, 1993.
17. Grant, J.E., et al., Analysis of dietary intake and selected nutrient concentrations in patients with chronic fatigue syndrome. J. Am. Diet. Assoc., 96(4):383-6, 1996.
18. Regland, B., et al., Increased concentrations of homocystine in the cerebrospinal fluid in patients with fibromyalgia and chronic fatigue syndrome. Scand. J. Rheumatol., 26(4):301-7, 1997.
19. Lapp, C.W. & Cheney, P.R., The ratinale for using high dose cobalamin (Vit B 12). The CFIDS Chronicle Physicians Forum, pp 19-20, Fall, 1993.
20. Dettori, A.G. & Ponari, O., Effeto antalgico della cobalamide in corso di neuropatie periferiche di diversa etiopatogenesi. Minerva Med., 64:1077-82, 1973. (In Italian)
21. Hank, A. & Weiser, H., Analgesic and antiinflammatory properties of vitamins., Int J. Vitam. Nutr. Res. (suppl)27:189-206, 1995.
22. Simpson, L.O., et al., Red cell shape changes following trigger finger fatigue in subjects with chronic fatigue tiredness and healthy controls., N.Z. Med. J., 106:104-7, 1993
23. Ali, M., Ascorbic acid reverses abnormal erythrocyte morphology in chronic fatigue syndrome. Am. J. Cin. Pathol., 94:515, 1990.
24. Ali, M., Hypothesis. Chronic Fatigue is a state of accelerated oxidative molecular injury. J. Advancment Med., 6(2):83-96, 1993.
25. Cox, I.M., et al., Red blood cell magnesium and chronic fatigue syndrome., Lancet, 337:757-60, 1991.
26. Howard, J.M., et al., Magnesium and chronic fatigue syndrome, Lancet, 340:426, 1992.
27. Seelig, M., Presentation to the 37th annual meeting, American College of Nutrition., Oct. 13, 1996.
28. Durlach, J., Chronic Fatigue Syndrome and chronic primary magnesium deficiency (CFS and CPMD)., Magnes. Res., 5(1):68, 1992.
29. Russell, I.J., et al., Treatment of fibromyalgia and chronic fatigue syndrome with Super Malic: a randomised, double blind placebo contreolled, crossover pilot study. J Rheumatol. 22(5):953-8, 1995.
30. Jessop, C., Super Malate and Chronic Fatigue, Fibromyalgia Network Newsletter, compendium#2, Oct 1990-Jan. 1992.
31. Toth, J., NK cells and their characteristics and immunogenetic aspects. Bratisl Lek Listy, 95(5):212-23, 1994.
32. Caligiuri, M., et al., Phenotypic and functional deficiency of natural killer cells in patients with chronic fatigue syndrome., J Immunol, 139:3306-13, 1987.
33. Cunha, B.A., Beta-carotene stimulation of natural killer cell activity in adult patients with chronic fatigue syndrome, TheCFIDS Chronicle Physicians Forum, pp 18-19, Fall, 1993.
34. Kuratsune, H., et al., Acylcarnitine deficiency in chronic fatigue syndrome, Clin Infect Dis. 18(suppl 1):S62-7, 1994.
35. Plioplys, A.V. & Plioplys, S., Serum levels of carnitine in chronic fatigue syndrome: clinical correlates, Neuropsychobiology, 32(3):132-8, 1995
36. Plioplys, A.V. & Plioplys, S., Amantadine and L-carnitine treatment of chronic fatigue syndrome, Neuropsychobiology, 35(1):16-23, 1997
37. Judy, W., South Eastern Institute of Biomedical Research, Bratenden Florida, Presentation to the 37th annual meeting, American College of Nutrition, Oct, 13, 1996.
38. Gray, J.B. & Martinovic, A.M., Eicosinoids and essential fatty acid modulation in chronic disease and the chronic fatigue syndrome, Med. Hypotheses, 43(1):31-42, 1994.
39. Horrobin, D.F., Post-viral fatigue syndrome, viral infections in atopic eczema and essential fatty acids, Med. Hypotheses, 32(3):211-17, 1990.
40. Behan, P.O., et al., Effect of high doses of essential fatty acids on the post viral fatigue syndrome, Acta. Neurol, Cand. 82(3):209-16, 1990.
41. Werbach, M., Textbook of Nutritional Medicine, Third Line Press, California, 1999.
42. Mills, S. & Bone, K., Principles and Practice of Phytotherapy, Churchill Livingstone Publishers, 2000.
43. Bone, K., A Clinical Guide To Blending Liquid Herbs, Churchill Livingstone Publishers, 2003.
44. Weiss, R.F. & Fintelmann, V., Herbal Medicine, Thieme Press, Stuttgart, 2000.
45. Spinella, M., The Psychopharmacology of Herbal Medicine, MIT Press, 2001.
46. Murray, M., The Healing Power of Herbs, Prima Publishing, 1995.
47. Walker, L.P. & Hdgson-Brown, E., Nature's Pharmacy, Reward Books, 1998.
48. Mills, S. The Essential Book of Herbal Medicine, Penguin, 1991.
49. van Wyk, B.E. & Wink, M., Medicinal Plants of the World, Briza Publications, 2004.