FLYING BC - January 2002
Page 9
______________________________________________________________________________________________________________________
Are You FIT to FLY?
The Diabetic Pilot: Prevention and Management - Part 1 by Dr. Randy Knipping
In 1995, Transport Canada published new guidelines for determining the aeromedical disposition of pilots with diabetes. At that time, only pilots with non-insulin dependent diabetes or Type II diabetes (DM-II) meeting specific criteria were made fit to fly with periodic special testing and reporting requirements. More recently, Type I or insulin dependent diabetics (DM-I) working as professional pilots in multi-crew settings, and selected air traffic control cases were approved.
The most important factor to understand with DM-II is that most cases are preventable and all cases can be effectively managed with a comprehensive approach to medical care and health risk modification. If you know of any pilot with diabetes who has stopped flying because they think they are unfit, then they need to read this article and get back to flying!
WHAT IS DIABETES?
The energy currency of the body is sugar, glucose to be more exact, and in order for this energy to be transported from our bloodstream to the "engines" within every living cell in our body, this same glucose has to cross over the cell wall. Insulin is a hormone produced by the pancreas gland just underneath the stomach and its principle function is to open a cellular "doorway" through which glucose can flow into the cell. Metaphorically speaking, insulin is like the key to a lock on this "door" without which the door remains closed and blood glucose accumulates (hyperglycemia) and the cell begins to search for alternative fuel sources or starves.
TYPE I DIABETES
Type I diabetes mellitus (DM-I) occurs when the pancreas, a digestive organ found just underneath the stomach, ceases to produce insulin, resulting in excessive levels of glucose (blood sugar) accumulating in the blood stream and a large number of resultant complications. DM-I is caused by an interaction between the human immune system and some sort of environmental stimulus, presumably a viral infection. This article will focus mostly on Type-II diabetes.
TYPE II DIABETES
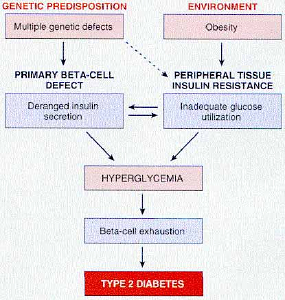
Type II diabetes mellitus (DM-II) occurs when body tissues especially muscles are unable to absorb glucose due to insulin resistance caused by an interaction between genetics and lifestyle, particularly central obesity, excessive carbohydrate consumption and inactivity. In addition, the production and release of insulin from the pancreatic beta cells eventually becomes impaired as well (see Figure 1). While DM-II results is somewhat less harm to the individual compared to DM-I, because of the larger number of people suffering from DM-II, this condition is actually one of the leading causes of serious chronic illness in the world today.
WHAT CAUSES TYPE II DIABETES?
If you would like to develop diabetes, here are the steps: first, pick your parents well. DM-II tends to cluster within specific families and there is evidence to support the role of a defective gene that predisposes an individual to diabetes. Next, engage in sloth and gluttony! Physical inactivity results in the gradual development of peripheral insulin resistance (the proverbial "lock" gets rusty through disuse atrophy. If you don't use them,
you lose them). Eating excessive simple carbohydrates, especially at night, and developing central obesity (a pattern of obesity where fat is predominantly deposited in the belly) then gradually results in defective glucose metabolism.
At first, the pancreas compensates for peripheral insulin resistance by pouring out more insulin into the bloodstream. Eventually, the beta cells in the pancreas become metabolically exhausted and blood sugar begins to rise after every meal.
HOW DO I KNOW IF I HAVE DIABETES?
Many people think that if they feel good, they are healthy. This is similar to thinking that if my aircraft engine is not making any noise, it must be working perfectly well. In the case of diabetes, it is this misconception that results in many pilots experiencing complications long before they develop any symptoms of diabetes. More than 50 per cent of patients diagnosed with diabetes already have evidence of organ damage at the time of diagnosis.
LOOK FOR DIABETES BY ASSESSING HEALTH RISK FACTORS FIRST
Early recognition and management of Health Risk Factors (HRM) for diabetes are as important to keeping you flying as regular preventive maintenance inspections of your aircraft. Monitoring weight, central obesity, physical activity, family history and
by Dr. Randy Knipping


